By Jerome Burne, health journalist and author
The trouble with healthy lifestyle advice is that it is so boring. At least the official medical version is. “Eat less (probably low fat) and move more” is one possible summary, along with all the same-old, same-old about not smoking, more fruit and veg, checking cholesterol and blood pressure levels and drinking moderately.
All unexceptional, although personally I’d avoid the checks that are usually a prelude to statins or blood-pressure pills and I think low fat advice is daft, but the package is about as alluring as warm underwear and sensible shoes. This is a tragedy not just for your health — who wants to follow boring advice? — but because the latest research on staying healthy as we get older is absolutely fascinating.
Whodunnit?
“The butler did it” is the whodunnit cliché but it’s a useful metaphor for pinpointing exactly why rates of our three major chronic killers - diabetes, cancer and Alzheimer’s - are soaring and threatening to overwhelm western health services.
In this story the butler is the hormone insulin, best known for appearing at the end of every meal and clearing the extra glucose out of the blood stream and into storage. What could be more butler-like than that?
His motivation is the excessive demand being put on him by our current high carb diet that’s transforming him from a loyal and devoted servant into a killer who’s ever-present as these diseases develop. The new secret to healthy living is not boring diet and exercise — but making sure your insulin butler has a lazy life.
Exposed in 4 chapters
The story of how insulin’s secret life as a serial offender was uncovered comes in four chapters: The Hungry Rat, The Methuselah Worm, The Dwarves of Ecuador and The Insulin-Loving Brain.
There is nothing new about the link between raised insulin and diabetes. Eating a diet packed with sugar (from junk food, processed convenience foods, refined cereals, confectionery, baked goods and heavy fruit consumption) keeps pushing up the amount of glucose in your blood after every meal. The effect is to force insulin to work overtime as it turns the extra glucose into fat and sweeps it away into storage.

Junk food: one of the sugary culprits loading your blood with glucose
And gradually things start to go wrong. The favourite depots – fat cells, muscles and liver – develop what’s called insulin resistance. They become deaf to insulin’s action as the door opener for sugar (i.e. energy) to enter the cells. You have to keep making more and more insulin before they will open up and make space, but all that circulating sugar that's not burnt as energy has no where else to go except the fat store!
The rising insulin levels can then start to affect the blood vessels of the heart and extremities such as the eyes and the feet, leading possibly to blindness and amputations.
So far, so familiar. But what happens when the blood levels of insulin and glucose are low? Is that necessarily linked with being healthier? In fact it is and the way to achieve it is very simple – just eat less. In more scientific circles, this is referred to as calorie restriction (CR).
Chapter 1: The Hungry Rat
Researchers have known for 70 years that feeding lab rats and other animals the human equivalent of 1200 to 1500 calories a day kept them super healthy with low levels of cholesterol and fats in the blood and, crucially, low levels of insulin. They also lived for between 20% and 40% longer (For more details see: Michael Ristow & Sebastian Schmeisser’s paper (Free Rad Bio Med. 2011; 51: 327-336) and David Stipp’s The Youth Pill (2010).
Chapter 2: The Methuselah Worm
For some time, nothing particularly practical or useful to humanity was done with the discovery of the crucial role of CR. That began to change in the 1990’s when geneticist Professor Cynthia Kenyon and colleagues at the University of California San Francisco found out why CR has this remarkable effect.

Cynthia Kenyon, University of California San Francisco
The secret lay in what it did to a gene that controlled insulin and a related growth hormone IGF-1 (insulin growth factor -1). Keeping these two damped down made animals like the nematode worm Caenorhabditis elegans long-lived and very healthy (Nature Genetics, 2001;28(2):139-45). Kenyon herself started following a low glycaemic diet herself as a result.
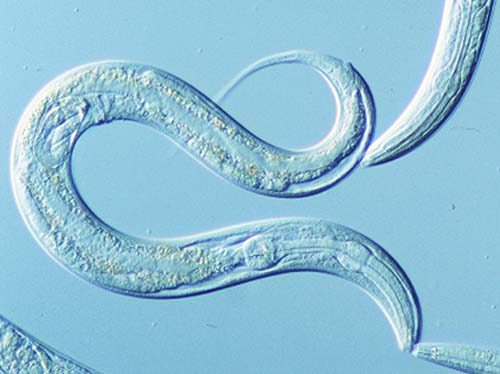
The nematode worm Caenorhabditis elegans
Chapter 3: The Dwarves of Ecuador
But how do we know keeping insulin damped down is likely to have a long-term effect on humans? This is where a remarkable natural experiment involving a community of Ecuadorian dwarves comes in. They have a mutation in the same gene that Kenyon had found. This is why they don’t grow properly early on but it also ensures they always have low insulin. The amazing overall effect is that they are generally healthy and specifically never get diabetes or cancer.
“Other members of their families who don’t have the mutation are a normal size and suffer from diabetes and cancer at a normal rate,” says Professor Valter Longo, a gerontologist at the University Southern California, Davies whose research describing their unique metabolism was published last year (Sci Transl Med. 2011; 3(70): 70ra13).
“What points the finger at insulin is that many of the dwarves are obese and have quite high levels of blood sugar yet still they are free of cancer and diabetes,” he says.

People with a certain kind of dwarfism in Ecuador seem immune to cancer, diabetes, age-related diseases
But why cancer? The link with diabetes, high blood sugar and insulin makes sense but how does cancer fit the picture? In fact scientists have known for some time people with diabetes are more likely to get cancer. The dwarves provide some valuable new clues about what may be going on.
In fact insulin, faithful butler that it is, doesn’t just clear away after meals. Having high insulin tells your body that food is available so now is a good time to do things that need energy like growing.
That’s vital when you are younger but more risky as you get older, because growth comes with a greater chance of mutations and the kind of damage to DNA that is linked with cancer.
“Insulin growth hormone turns on growth promoting pathways in the body,” says Longo. “The dwarves have it turned right down and so do genetically engineered mice, which also have a big drop in their risk of cancer.” Researchers studying ageing are now looking for ways to get the same effect with drugs.
Further clues
More clues about how the diabetes-cancer link works has been showing up at Harvard University where Professor George Daly, a stem cell transplant expert, studies proteins that cut cancer risk by slowing the rate cells grow. (Nat Genet. 2010; 42(7):626-30).
“We were amazed to find that they also had a remarkable effect on the way mice process sugar and on their risk of developing diabetes,” he said.
Chapter 4: The Insulin-Loving Brain
The big new idea is that, just as high levels of blood sugar and insulin can raise the risk of diabetes and cancer, insulin is now being implicated in Alzheimer’s. The brain runs on glucose and uses insulin to lay down memories and grow brain cells in areas like the hippocampus, a key player in memory (see article by Bijal Trivedi in New Scientist, 3 September 2012).
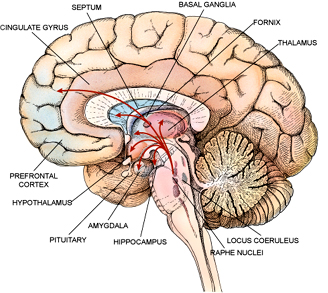
The human brain
Problems start when a typical Western diet, rich in sugar, creates insulin resistance so more and more of it is needed for the same effect. Last year a small study looked at the spinal fluid in healthy volunteers who had been on a junk diet for only four weeks. (Arch Neurol. 2011; 68(6):743-52).
They had a raised level of the markers for the damaged protein 'plaque', a classic marker for Alzheimer’s, that can build up for years without causing symptoms. Other research is pointing in the same direction.
There is still a lot of work to be done to understand all the connections here. Not everyone with diabetes gets cancer and you can have Alzheimer’s without diabetes and vice versa.
Screaming need for more science
But the discovery of a possible lifestyle link between three chronic killers should, in a rational medical system focused on patients rather than profits, trigger major research programs into how best to influence it most effectively. Do different people benefit more from certain types of insulin lowering diets or from different exercise regimes?
Knowing that specific lifestyle changes can affect the genes controlling insulin pathways makes targeted lifestyle interventions a possibility. Finding out how best to do that should surely be a priority?
And the insulin link is not the only one. Mineral, vitamin and phytonutrient deficiencies may well play a part in all these conditions along with stress and other psychological states.
At the moment, though, a co-ordinated research program to investigate these possibilities is mere fantasy. Who is going to pay for it? So the search is endlessly focused on the new drug target that will affect insulin and other pathways. Claiming that constitutes evidence-based medicine has to be a major error. Left uncorrected will most likely allow the butler to get away with it.
More on Jerome Burne

Jerome Burne will be talking about the links between ageing well and insulin at CAMExpo at Earl's court this Saturday, October 20th at 3.00 pm.
His book 10 Secrets of Healthy Ageing written with Patrick Holford has more details on genes and insulin and lifestyle and is now on sale.
Jerome’s blog, Body of Evidence, is about how the current system of evidence-based medicine that needs a major overhaul.







Comments
your voice counts
18 October 2012 at 7:48 pm
Untill it is recognized by citizens that they are being exploited by the big corporate medical system there will only be low funding for important research. The funding must come from pure sources not corruptable by the medical industrial complex. They have their dirty money everywhere and as long as the sheeple continue to sleep...nothing will happen.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences