Content Sections
The NHS turns 70 tomorrow (5thJuly 2018). Created in 1948 to provide free and universal access to healthcare, it’s regarded as one of Britain’s most significant achievements in the last century.
The big question is: how much longer can it survive on its present course?
Founded to provide universal, equitable, comprehensive, high quality healthcare free at the point of use, funded largely by general taxation, the NHS is unique globally. Since its inception, rapid changes in society and societal health have pushed this ageing service into becoming a disease management system that is at breaking point. With the current levels of funding, the present disease burden and the expectation of the public, the NHS – along with its 1.7 million staff – can no longer cope.



One of the largest employers in the world
Among its strengths is the NHS’ sheer size. It employs a staggering 1.7 million people in the UK making it the fifth largest employer in the world (Fig. 1) and easily the biggest in the UK.
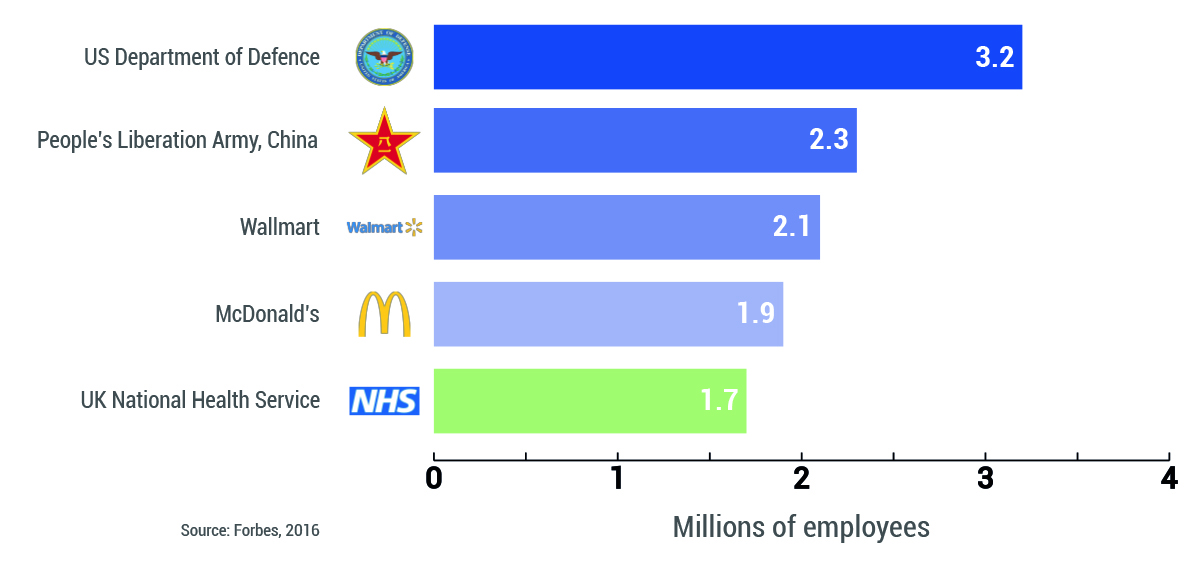
Figure 1. Top five employers in the world
Source: Nuffield Trust.
A Constitution – for the people of Britain
The NHS Constitution opens with a powerful statement that isn’t common to the healthcare system of most countries:

Interestingly, it is the Constitution only of NHS England, “the devolved administrations in Scotland, Wales and Northern Ireland [being] responsible for developing their own health policies".
The Constitution establishes bold aspirations:
So, what are the principles, values and pledges?
The NHS was originally founded on just 3 core principles, these being:
- That it meets the needs of everyone
- That it be free at the point of delivery
- That it be based on clinical need, not ability to pay
Its principles have since expanded to seven. They are:
- The NHS provides a comprehensive service, available to all
- Access to NHS services is based on clinical need, not an individual’s ability to pay
- The NHS aspires to the highest standards of excellence and professionalism
- The patient will be at the heart of everything the NHS does
- The NHS works across organisational boundaries
- The NHS is committed to providing best value for taxpayers’ money
- The NHS is accountable to the public, communities and patients that it serves
Coupled with these 7 principles, and also laced into its Constitution, are a further 6 values:
- Working together for patients
- Respect and dignity
- Commitment to quality of care
- Compassion
- Improving lives
- Everyone counts
If that wasn’t enough, the NHS Constitution makes a number of pledges to patients and the public:
- Patients come first in everything we do.
- You have the right to receive care and treatment that is appropriate to you, meets your needs and reflects your preferences.
- You have the right to accept or refuse treatment that is offered to you. You have the right to be given information about the test and treatment options available to you, what they involve and their risks and benefits.
All in all, the NHS’ Constitution hits so many of the right notes. But it’s not perfect. For example, it makes only a single mention of the word ‘prevention’. The Constitution states that it should “involve patients, their families, carers or representatives fully in decisions about prevention, diagnosis, and their individual care and treatment.”

The lack of adequate focus on disease prevention may indeed be the origin of the NHS’s biggest problems, given the scale of the current preventable disease burden.
Facing the challenge
The challenges being faced by the NHS today are myriad and complex. They include:
- The NHS has become a disease management system for the epidemic of preventable chronic diseases caused by such things as poor diet, drug and alcohol abuse, physical inactivity, psycho-social stress and smoking
- It is battling with an increasingly ageing population – something that should give cause for celebration. Unfortunately, many suffer from multi-morbidities, often requiring multiple interventions from a disjointed service along with a poly-pharmacy of drugs
- Past successes with antibiotic treatment of infectious diseases have created a public expectation of miracle cures and a ‘pill for every ill’
- Antibiotic failures caused by antibiotic-resistant strains of pathogen are leading to a resurgence of hard-to-treat infectious diseases
- Waiting lists grow as preventable chronic diseases spiral out of control
- There are no adequate solutions offered for the growing autism and mental health burden
- Staffing shortages coupled with increasing demands is putting severe pressure on existing staff and resources
The need for a revolution
There is no magic bullet that can resolve some of biggest issues the NHS faces linked to the chronic, autoimmune and mental health disease burden. No amount of technology, artificial intelligence or even money will fix these issues when the solutions to them are outside the scope of NICE guidelines.
To become a system that’s truly person-centred, focused on disease prevention and health promotion, the NHS needs to fundamentally change from being a disease management system to a health creation system. It must be a system that’s truly sustainable and fit for future demands.
None of this can happen until a much higher level of individual engagement happens, to the point that each individual truly feels in the driving seat of their own health. The current system is disempowering for many and it fails to address the upstream causes of disease. There is a clear need for a common language that can be used between the public and all modalities of health professional.
‘Lifestyle advice’ is recognised by NICE as being appropriate for first line treatment of type 2 diabetes, but the guidelines are so broad and vague as to be of little use in practice.
Nutrition is beginning to be taught to medical students – but this initiative hasn’t been spawned by the NHS, it’s been driven by medical students who are trying to fill critical gaps in their training.

ANH’s contribution
We’ve been working for years on how sustainability can be applied to health, how to pay more than lip service to prevention, and how people can regain health sovereignty. All of these approaches are being incorporated into our ‘Blueprint for health system sustainability in the UK’ to be published later this month.
It’s not about applying any new fixes to the NHS. It’s about how we can work on dramatically improving self-care. But also how we can work in a collaborative and a participatory manner with a much broader pool of health and fitness professionals. It’s about a bottom-up solution, not a top-down one.
Taking the pressure off the NHS by lessening the burden of preventable disease is a goal that almost everyone shares, possibly with the exception of those who profit from either creating or selling products or services to a diseased population.









Comments
your voice counts
05 July 2018 at 9:58 am
The NHS since its first inception was a fantastic idea , but what the false media keep pushing is telling you its "FREE" , well that is not the case as most know because you pay for it by your NI contributions which adds up to a staggering amount .
The huge problems now are huge delays for desperate operations and what with people being over medicated and wrongly diagnosed we have a health time bomb waiting to implode . Many health workers now have to question wether they become whistle blowers to tell us how it really is , most of them are hard & dedicated workers but the system they are under is appalling and ineffective . Managers of the NHS now need to implement a new system that will include integrated medicine and most importantly of all a program to make sure people have the knowledge of how to treat themselves for minor problems with many natural cures which are available , so an integrated system of preventative medicine is needed to avoid the impending disaster . Most will have heard of the "prevention of an illness is better than the cure ",and this is why I would like to see much much more done in the preventative fields . "But" as there always is one we have massive drug companies that want their pounds of flesh and will do anything to avoid "other " methods of prevention and cure , this is a huge battle but the good will always win and we have to believe that we can win . Here's to a much better NHS in the near future .
06 July 2018 at 12:35 pm
Still reeling from McDonalds bring 4th biggest employer?! Great article.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences