By Rob Verkerk PhD, founder, scientific and executive director
I won’t ever forget the way in which one of the world’s most influential nutritional epidemiologist’s responded to a question from the audience at Swiss Re’s 2018 summit at its Centre for Global Dialogue just outside Zürich, Switzerland.
Amanda Atkins, a filmmaker, is passionate about telling the story and that of thousands like her who have reversed diabetes via a very low carb diet. She challenged Prof Dariush Mozzafarian, a cardiologist and epidemiologist from Tufts University in Boston who has a major influence on government healthy eating guidelines around the world. Mozaffarian had already given a lecture suggesting that low carb is irrelevant as it only looks at one of the three macronutrients, and ultimately quality is much more important than focusing on macronutrient proportions.
Amanda’s challenge went something like this: I might be n = 1, so I know my case won’t influence your thinking. But I’m talking to thousands of others who’ve had the same experience and completely reversed their type 2 diabetes without drugs and now have HbA1c levels that are in the normal range – all with nothing other than a low carb/high fat diet. Mozaffarian was unmoved and simply dismissed her – to the horror of most of the audience, most being clinicians who had witnessed the benefits of low carb diets in their patients many times over. Mozaffarian’s stubbornness was borne out of a blind reverence to published clinical epidemiological studies. Bottom line, there were none of high quality in his view that evaluated what we might think of as healthy low carb diets. Mozaffarian was also aware that some of the world’s longest lived populations, such as the ‘Blue Zoners’ from the Sardinian mountains or Okinawa in Japan consume relatively large quantities of carbs, while the Inuits who eat high fat diets die young. These were the very kind of controversies that Swiss Re, one of the world’s largest re-insurance companies, aided by an impartial medical journal, the BMJ, wanted to get under the skin of.
So – how far have things moved on in two years. This year’s summit did not allow us to enjoy from Swiss Re’s Centre for Global Dialogue the breath-taking views of Lake Zürich and the Alps. The conference was now virtual, courtesy of Covid, and ran for two days, each day with 3, punchy one-hour segments.
I bring you here some feedback on Day 1 that I was able to attend, but you’ll find below also videos of the Day 2 sessions. Day 1 kicked off with a wrap-up of lessons learned from the 2018 Food for Thought summit, and the other two segments each dealt with a thorny nutrition topic: type 2 diabetes reversal and salt in the diet, respectively.
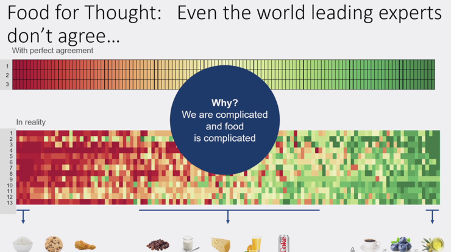
Prof Tim Spector reminded delegates of the complexities of nutritional science that contribute to the many ongoing nutritional controversies.
For those with a desire to view all of the segments in Days 1 and 2, you’ll find the recordings at the base of this article for your viewing and educational pleasure. For those who’re short of time, let me give you the take homes I felt were most relevant (albeit with some of my own spin on them) from the Day 1 sessions:
- Consensus over many areas of nutrition is a long way off. Getting scientists to agree over what represents a healthy approach to eating is never going to be easy because we’re all individuals, each with unique genetics and microbiomes, that have experienced the world and eaten foods in ways that are different from others, so setting up unique patterns of genetic expression. The long and short is that two people will always respond to the same food differently. That means studies on big populations – the stuff that epidemiologists obsess about that form the foundation of government eating guidelines – may have little relevance to an individual.
- Changing views of what comprises evidence in nutritional science. What’s considered relevant evidence is expanding and there is a general sense that randomised controlled trials (RCTs), that remain the gold standard for pharmaceutical interventions because they are statistically powerful and have high internal validation, have limited value when it comes to nutrition. The reasons for this are complex, but one of them is that you can’t run a true control – which would typically mean avoiding exposure to the treatment in the control arm. That’s (believe it or not) because we all need to eat, including those in the control arm of a clinical trial. If you then try to manipulate a diet, giving a bit more of some nutrients while removing others, you enter the world of complex interactions, matrix effects and lots of confounding. So it all gets very messy. Big data analytics and machine learning are increasingly viewed as the emerging approaches that can help us to make sense of real world data derived from people living real lives and they have the potential to give us crucial additional evidence for what is good for particular individuals and sub-populations.
- There is an increasing drive to move away from categorising foods as ‘good’ or ‘bad’. Unless, of course, they are very high in refined carbohydrates including sugar, transfats, artificial ingredients, etc. That’s because context and quality can change whether a food is good or bad for us. Let me give you an example using spaghetti bolognese as an example of a dish, the healthiness of which we’d like to know more about (this example was not raised in the Swiss Re discussion). Someone who’s just run a marathon will help to reinstate their depleted glycogen more quickly if they eat a plate of spaghetti than if they eat a low carb steak. That same spaghetti eaten every night, especially late at night in the absence of vegetables or plant foods, by a sedentary person, could push that person into metabolic disease like type 2 diabetes or obesity. If the spaghetti is overcooked, it becomes very high glycaemic and will be more likely to contribute to insulin resistance, the precursor to diabetes. If it’s cooked al dente, as served in Rome, it’s low glycaemic and will produce a much less pronounced blood sugar response. If the meat is from industrially produced beef, it has very little in the way of tomato concentrate in the sauce, and there’s no vegetables or salad served alongside, it will on most measures be less healthy for most people than a bolognese sauce made with grass-fed beef, lycopene-rich sundried tomatoes and passata, and plenty of fresh rosemary and a dash of resveratrol-rich red wine, with a pesticide-free wild rocket salad on the side. If the person is gluten-sensitive or, worse still, a coeliac, the spaghetti will always be a bad, or very bad, choice, regardless of context. That I hope, by example, gives some feel for why quality and context are so important.
- Type 2 diabetes is definitely reversible with diet alone. For me, this was the big progression since the 2018 summit – even the likes of Mozaffarian has come some way around to accepting it. It was great having Michael Mosley moderating – coming from a place of knowledge both as a doctor and as someone who’d reversed his own diabetes by going low carb along with intermittent fasting and making a mint out of his Fast (5:2) Diet book. I was a little disturbed about some of the views on causation, however, especially coming from eminent Newcastle University low calorie diet scientist Prof Roy Taylor. Prof Taylor was convinced that the evidence he and his team put forward over a decade ago that diabetes was caused by fat build up in the liver, and subsequently in the pancreas, was the cause of diabetes. My thoughts were that Prof Taylor was not looking sufficiently upstream, at the cause of the cause, or the cause of the cause of the cause – as brilliantly elucidated by the Australian doctors, Garry Egger and John Dixon. Another way of looking at it is that it is a change in hormone levels that contribute to the build-up of intra-organ fat. As pioneering, UK low carb GP, David Unwin, proposed, insulin is the key fat storage hormone, so when elevated in the bloodstream because of the development of insulin resistance, it’s insulin that pushes fat into the liver. There may be socio-economic drivers for the development of eating patterns that contributed to the hormonal dysregulation of appetite (grehlin, leptin) and energy metabolism (insulin, glucagon, incretins, adiponectin, etc.) that resulted in the fat build up that Roy Taylor has spent years looking at using magnetic resonance imaging (MRI). There may be trauma, food addiction, domestic violence, or any manner of other stressors that played their part that would never have been seen by an MRI scanner. We have to look upstream if we’re to help resolve downstream problems and the person who knows most about what happened upstream is typically the body’s owner, not a white-coated doctor. And looking upstream as far as the eye can see, and helping individuals to assess multi-system function while being fully aware of the ecological context in which they exist are two of the major pillars of our blueprint for health system sustainability project. Roy Taylor, as a low calorie rather than low carb protagonist, redeemed himself during the discussion in my eyes when he said one of the most useful pieces of advice he’s found for patients has been to tell them to “eat normally during the day but don’t put bread, pasta, rice or potatoes on your plate for your evening meal.” That sounds like low carb advice to me.

The diabetes reversal panel
- Carbohydrate intolerance is a driver for type 2 diabetes. This point was wonderfully made by Prof Arne Astrup from the University of Copenhagen. Insulin resistance from repeated over-exposure to insulin, in turn the result of elevated blood sugar — raised circulating insulin and blood sugar being the two hallmarks that lead to type 2 diabetes — doesn’t just affect muscle cells. It also affects the brain. Astrup proposed that when the brain doesn’t get the glucose, it fails to be satiated — and the afflicted individual eats and snacks more and the vicious spiral commences. Importantly, those who are on the spiral, who are suffering dysregulation of their hormonal, energy balance and appetite regulatory systems, respond to carbohydrates differently to those who are functioning normally. In essence, those with metabolic disease typically become increasingly carbohydrate intolerant, and that’s a major reason why low carb, intermittent fasting approaches (that often contribute to people eating less food overall including less carbohydrate) work so well in those who have already started their journey into metabolic dysfunction. It’s not too late to U-turn, but don’t wait for governments, Big Food or, sadly, most doctors, to tell you what you should be doing. Fortunately the number of exceptions to this lamentable situation is growing, not declining. But we also know there are other factors that control satiation and trigger continued eating when ample energy is onboard (as subcutaneous fat), such as the triggering of reward pathways in the brain by taste receptors exposed to high sugar/high fat foods.
- Time to ditch the calorie. It was a revelation to sense the support for the notion put forward by Prof Tim Spector when he voiced his disdain for calories as a useful measure for assessing dietary impacts on health. He said you can’t measure them easily, and they are not meaningful as a determinant of health. He said we should ditch our obsession with calories on labels and focus on quality and personalising nutrition so it benefits the individual and their specific microbiome
- ‘Less is better’ for salt is dangerous. The third segment opened the can of worms of government salt recommendations. It was great to hear what I thought was a huge amount of common sense and accurate scientific interpretation coming from Martin O’Donnell from the National University of Galway warning of the dangers of consuming too little salt (less than 2.3 grams of sodium = 5.75 grams of salt per day), given the well observed U-shaped relationship of sodium intake to hypertension and cardiovascular events. He also emphasised the importance of high potassium, the main source of which in the diet is non-starchy vegetables. Exactly right, we’d say. Although you’ll see Graham MacGregor from the Wolfson Institute who has been one of the most outspoken campaigners for salt reduction in the UK wasn’t so sure. He felt that governments’ public health recommendation to consume less than 6 grams of salt (=2.4 grams sodium) a day was still the right thing to do, failing to appreciate that this target puts people so close to threshold at which risk increases and gives the impression less is better or that zero is optimal. MacGregor also argued that current levels of salt intake are 100 times greater than that during the majority of our evolutionary development.
- Processed foods are killers. If there was one point about there was apparent consensus, this was it. Big food’s processed offerings are killing people, slowly but surely. Much of the epidemiological data (e.g. the PURE study for example) is clouded or confounded by differing amounts of processed food consumption. But in studies in which the amounts of processed foods are taken into account, there is a consistent view that they’re bad for health. Arne Astrup was asked about saturated fat – and reflected the current state of the science, as one would expect: while saturated fat intake can increase LDL cholesterol, there is little evidence that large particles of LDL, that are the main LDL fraction that are associated with diets with higher saturated fat intake, contribute to an increased risk of heart disease and mortality. Equally, there’s no good evidence that increasing saturated fat intake increases amounts of small dense LDL, which is the fraction of LDL that is subject to oxidation and is associated with an increase in atherosclerotic plaque formation and subsequent cardiovascular events.
Closing words
It is the complexity of nutritional science, still an emerging discipline, that makes it so hard to achieve consensus. Big differences in results of studies on individuals are seen as compared with those on populations. Interactions are multi-layered (and multi-trophic), between animals, plants and microbes, along with all of their respective genes. They all function, in turn, in incredibly diverse and often changing environments, with and without highly variable amounts of human interference. All that before you throw in the effects of economics and politics.
And people wonder why there are so many different views on what constitutes a healthy plate of food.
Dive in below to the recordings from Food For Thought 2020 – and congratulations to Swiss Re and BMJ for making the summit happen again, albeit virtually.
RECORDINGS OF DAYS 1 AND 2 SESSIONS, FOOD FOR THOUGHT 2020 (virtual summit)
Day 1
Day 2
>>> Back to Reverse Diabetes Naturally campaign
>>> Back to ANH International homepage








Comments
your voice counts
03 July 2020 at 7:22 am
Absolutely nothing will change as long as governments - knowingly and deliberately - endorse poisoning and chemicalization of crops and food products by corporations, such as Bayer, Nestle, etc. Synchronised, global action is needed... desperately.
04 July 2020 at 11:14 am
Agreed Ela! action in those areas is past desperate. Its Crucial for all human beings. Mental and Physical health.
When artificial meats" are in the Hamburger shops (& Gates has a major share in Mc Donalds in Brazil especially), and now BREAST milk is to be (possibly) put on shelves, its critical, crucial to get this sickness fixed.
Countries such as Australia ,that has "permitted" GMO foods, MUST pass Legislation that Produce that is sold to the public, and said food is LABELLED CLEARLY that the produce on Sale is a GENETICALLY MODIFIED PRODUCT. and/or is a hydroponic produced vegetable, this is long overdue. There is enough deception with the over-farming of the soils in Australia, then the - up to 21,000klms that the food can be transported in a refrigerated truck.
When I am back in Australia I make sure I do not go to certain Supermarkets as the air conditioning for the whole store is so cold, not only the chiller area that the produce is placed in, usually the smaller country supermarkets, where people do not have another produce store to buy from.
I note that in Italy there is a small space for chilled produce (most from the local region, and in Japan nearly every item (fish-NOT farmed Salmon), vegetables, fruit, etc.,) in a store is incredibly fresh and a delight to look at, and a pleasure to shop in, the varieties of fish, mushrooms, and other produce. The very small space left in the store is for cleaning items. If you want hairbrushes, newsagent type items & other non-food goods you go to those stores, NOT the food store.
When I have been in Italy or Japan I am so healthy, when in Australia I show physical signs of poor quality food intake. - not good for Auto Immune person, children or anyone. Making us more susceptible to health problems. I used to grow my own food, but having to be Doctor to my formerly International-Career sons, due to the lack of knowledge of the medical world in diagnosing and treating Auto Immune disorders that I became a Researcher and Doctor for us all and it worked.
Individuals MUST write to their Governments. As a former very senior Federal Government Minister said 35 years ago to me. "one letter is equal to 100 letters from the Public".
13 August 2020 at 3:24 pm
Just one point on the spaghetti bolognese point - there is actually good research suggesting that those on low-carb or keto diets are able to replenish glycogen stores just as fast as those who consume carbs after exercise.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences