Adam Smith
Science and Communications Officer, ANH-Intl
Vaccination is one of the most controversial topics in the modern world, about which the public is asking many, as well as more and more complex, questions. Unfortunately, with the enormous amount of vaccine-related misinformation and deliberate disinformation out there, many are finding it difficult to get straight answers. And this is what this Q&A is about!
Below are 7 commonly asked questions on vaccination, all of which are linked to our answers. In each case, we have linked to further information where readers can find more detail if you so wish. We hope the answers will help you to make an informed choice about whether or not to vaccinate – as ANH-Intl is all about choice in vaccination.
The questions
1. Does vaccination equal immunisation?
3. Are you risking ‘herd immunity’ and acting selfishly if you choose not to vaccinate your kids?
1. Does vaccination equal immunisation?
In short: no, not by any means. But let’s back-track a little bit.
The idea behind vaccination is quite simple: that introducing into the human body weakened or inactivated pathogens, or parts of pathogens, that would normally cause disease if fully live, will ‘prime’ the immune system to recognise the disease-causing agent upon future encounters. This priming puts the immune system on permanent lookout for that particular threat, allowing it to mount a strong immune response to the invading pathogen and fight off the infection. This process is meant to mimic natural adaptive immunity, in which the body deals with a particular pathogen and becomes immune to further infection for life.
Logically, then, if this theory were correct and vaccinations work as they are meant to, infectious disease rates would drop to near zero among vaccinated populations, with batch variation accounting for the unfortunate few who still contracted disease. Dreaded conditions like tuberculosis, diphtheria and polio would become diseases of the past (see below). Vaccinated populations would be healthier than ever before (see below), removing enormous pressure from health services in those countries. Vaccination would, in short, be one of the greatest boons ever known to humankind, and all infectious diseases that are subject to childhood vaccinations would be relagated to the history books.
Also perfectly logically, in the era of supposedly evidence-based medicine, one would expect vaccines to be backed up with gold-plated science. Anything recommended for infants as young as 2 months, or even 1 month, as part of a schedule that continues throughout adolescence and beyond and which some pay for with their taxes must be the safest, most effective thing in the world – mustn’t it?
Unfortunately, this is where logic begins to unravel. Anyone, it seems, who forensically examines the medical literature in search of evidence that vaccines actually confer the wonderful benefits claimed for them is disappointed. Recently, Gary Null PhD took a wide-ranging look at the literature on vaccination in general, and came to a startling conclusion: “Of thousands of articles in the peer-reviewed literature on immunology nowhere can we find gold standard, double blind, placebo controlled studies that prove that any vaccine or combination of vaccines can be shown to provide lifelong immunity and safety to any individual.”
Even a brief look at the literature reveals numerous examples of vaccine failure – when vaccination either does not confer immunity from day one, or when the immunity fades after a short period of time – including measles, haemophila influenza type B (Hib), hepatitis B and pertussis (whooping cough). Infectious diseases like measles, mumps and chicken pox are recorded as occurring in highly vaccinated populations.
The very fact that so many ‘booster’ vaccinations are recommended by authorities these days speaks volumes about the inability of vaccines to confer long-term immunity. However, it appears that many within the orthodox medical establishment, governments and media alike would have us believe otherwise: that vaccinations not only cause instant, permanent immunity to whatever is vaccinated against, but that immunity is impossible without vaccines. This thinking leads directly to the heavy childhood vaccination schedules increasingly encountered in the industrialised world.
2. Polio, measles, diphtheria and whooping cough often get held up as the vaccine success stories. Is this the case?
It’s very difficult to argue with figures showing that death rates associated with these infectious diseases have plummeted since the advent of vaccines. However, a closer look at the statistics reveals a different story.
Polio
The official narrative on polio is that, between them, vaccines containing live attenuated and killed forms of the polio virus have reduced the global incidence of polio from 350,000 in 1988 to a mere 1,352 in 2010. Polio is no longer seen in the industrialised world, a victory that many attribute entirely to the vaccines.
However, international mortality statistics from 1981 show that polio incidence in the USA and UK was already on the decline before any vaccine was introduced [1] – by 47% and 55%, respectively, between 1923 and 1953, when the first vaccine was introduced. Polio epidemics also ended in countries that did not systematically vaccinate their citizens [1]. Not only that, but the standards for reporting polio were altered at the time of the vaccine’s introduction. Aseptic meningitis and coxsackie virus infection, for example, were reported as polio before the advent of vaccination, whereas they were usually reported separately afterward – greatly reducing the apparent incidence of polio [1].
Also reported under the banner of ‘polio’ prior to vaccination was a condition called acute flaccid paralysis (AFP), which itself covers several individual health problems, such as transverse myelitis and Guillan-Barré syndrome. Figure 1, sourced from World Health Organization (WHO) figures, shows that the incidence of AFP has rocketed relative to that of polio since 1996.
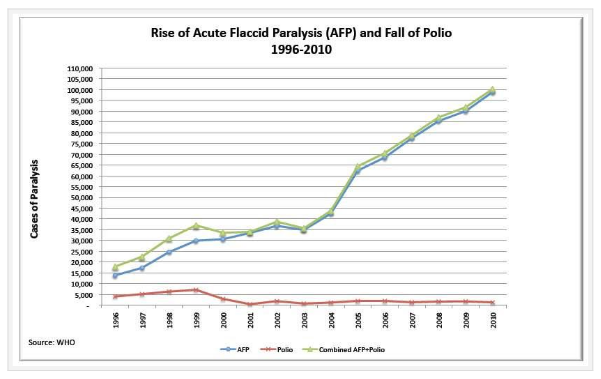 Figure 1. Rates of acute flaccid paralysis and polio, 1996–2010
Figure 1. Rates of acute flaccid paralysis and polio, 1996–2010
[http://drsuzanne.net/wp-content/uploads/2012/07/Smoke-Mirrors-and-the-%E2%80%9CDisappearance%E2%80%9D-Of-Polio-_-International-Medical-Council.pdf]
On a global scale, the WHO acknowledges that new wild forms of polio virus have emerged as a direct consequence of vaccination, making its initial goal of eradicating the disease by year 2000 impossible [1]. Some officials believe that this phenomenon could eventually see a form of polio virus appear in the Western hemisphere for the first time in decades [1].
Measles
The picture with measles is similar in some ways to that observed with polio: an official narrative that attributes amazing success to the vaccine, with published statistics entirely at odds with that assertion.
Data from Australia (Figure 2) show that deaths due to measles had declined by 99.5% in the 100 years prior to vaccination in 1970. It’s a similar picture in the UK (Figure 3) and USA (Figure 4), where measles vaccines were first introduced in 1968 and 1963, respectively.
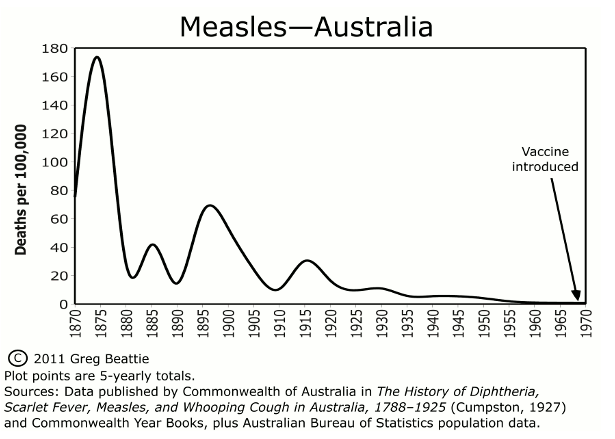
Figure 2. Measles incidence in Australia, 1870–1970
[http://vaccinationdilemma.com/historical-death-rates-diseases-vaccination].
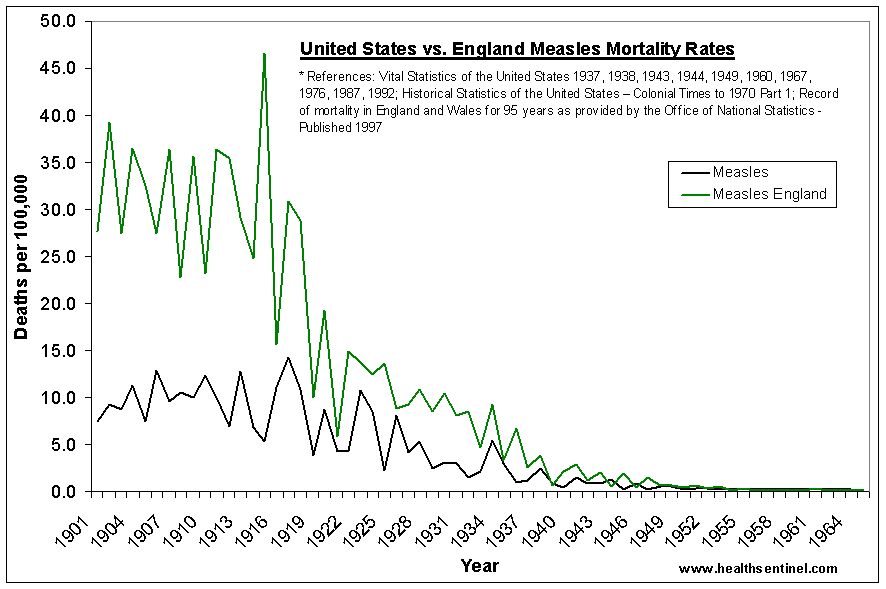
Figure 3. Reported measles cases and death per 100,000 population, USA, 1912–1917 [2].
[http://childhealthsafety.wordpress.com/graphs/#Meas_Mort_UK_USA]
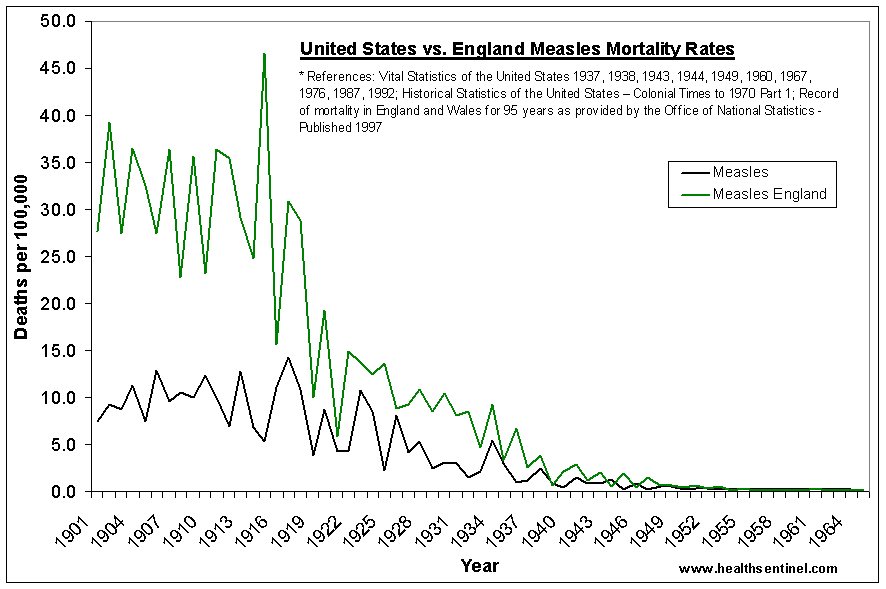
Figure 4. Logarithmic scale of measles mortality in England and Wales, 1901–1999 [http://childhealthsafety.wordpress.com/graphs/#Meas_Mort_UK_USA] (by Clifford G. Miller, for evidence in the Dr Jayne Donegan [http://www.thehomeopath.org.uk/wp-content/uploads/VaccinatableDiseasesTheirVaccines.pdf] General Medical Council hearings [http://www.jayne-donegan.co.uk/gmc], August 2007, Manchester, UK)
Diphtheria
Here, it’s a slightly different story. Although the official narrative is reliably pro-vaccine, the actual figures seem to show that diphtheria incidence decreased naturally over time, through a combination of reduced viral virulence and increased host resistance.
Whooping cough (pertussis)
Falling into the now-familiar pattern, the official story attributes enormous success to vaccination in reducing deaths from whooping cough – while Figure 5 shows that death rates had already fallen by over 90% by the time the vaccine was introduced.
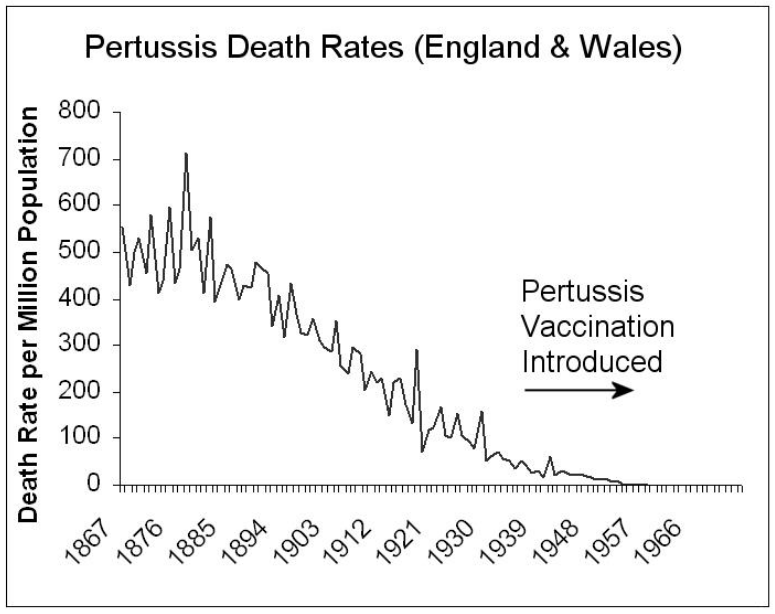
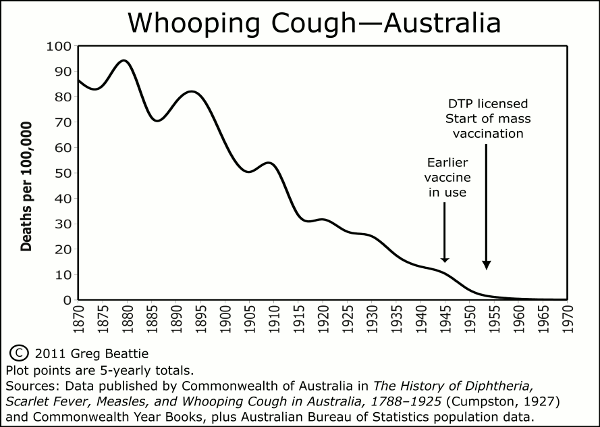
Figure 5. Historical mortality due to whooping cough (pertussis) in England and Wales (left) [http://www.thehomeopath.org.uk/wp-content/uploads/VaccinatableDiseasesTheirVaccines.pdf] and Australia (right) [http://vaccinationdilemma.com/historical-death-rates-diseases-vaccination], including the date of introduction of vaccination in both countries. Source of information for UK graph: Deaths/Population 1867–1900, Registrar General’s Annual Returns, 1901–1994, Twentieth Century Mortality CD-ROM, Office for National Statistics.
Of course, there's more to diseases than just whether or not they kill their victim! Vaccines that dramatically reduce the incidence of disease could doubtless be beneficial in terms of reducing suffering as well as the burden on the healthcare system. However, we are told over and over again by health authorities and many historians that vaccines are almost solely responsible for reduced rates of once-deadly infections, saving countless millions of lives in the process. We think it’s pretty clear that this is not the case, or the case, at very least, is greatly exaggerated. Factors such as improved diet, hygiene and sanitation, leading to improved host resistance, plus reduced viral virulence are likely to be more significant factors in many cases.
3. Are you risking ‘herd immunity’ and acting selfishly if you choose not to vaccinate your kids?
By making parents who question childhood vaccination on the grounds of their kids’ health feel guilty that they may be putting others at risk, ‘herd immunity’ is an extremely emotive argument in favour of childhood vaccination. The theory is that, if a certain proportion of any population is inoculated against a disease through vaccination, it inhibits the spread of that disease within the population. People who cannot receive vaccines for whatever reason, say on religious grounds or sensitivity to a vaccine’s ingredients, are thus protected from the disease by a high level of vaccination within society. It follows, according to herd theory, that parents who don’t vaccinate their children put the health of wider society at risk. Health authorities, media commentators and increasingly schools and parent-teachers associations, waste no opportunity to bash parents over the head with this message.
The key concept to bear in mind with herd immunity is that, however hysterical the coverage, herd immunity is only a theory. A plausible theory, but a theory nonetheless – and one that developed out of observations of natural immunity, not vaccination effects. Statisticians observed that populations were protected when sufficient members contracted the wild form of a disease, and subsequently acquired lifelong immunity. We simply do not know whether or not the same is true of vaccination in general or of particular vaccines, but we can certainly say this: discredit herd immunity, and a powerful supporting plank of vaccine theory vanishes into dust. So the vaccine manufacturers have a double motivation for pushing herd immunity, because it sells more vaccines and it helps to maintain an environment in which vaccines are considered essential for health.
Bearing all this in mind, it’s clear that parents who choose not to vaccinate their children should not feel guilty. Regardless of the propaganda, the evidence shows that unvaccinated children can catch infectious diseases from vaccinated children; and therefore, high rates of vaccination cannot effectively protect those members of society who are unable to take vaccines. This point alone puts a rather large nail in the coffin of herd immunity! Only widespread natural immunity is guaranteed to protect a society from infectious diseases, but since it relies on most citizens having healthy diets and lifestyles, we have a long way to go. Wouldn’t it be interesting if the pressure was on to have a healthy diet and lifestyle in order to increase natural immunity instead?
4. How much research has been done on the risks to a child undergoing the full, recommended vaccine schedule?
In a sane world, the answer would be go something like this: “huge amounts! No expense has been spared to prove beyond a shadow of doubt – as much as is possible through the scientific method, at least – that the currently recommended childhood vaccination schedules are safe for our children.” After all, to give two examples, children in the USA are given 49 doses of 16 vaccines before age 6 and UK kids are vaccinated against 10 different diseases by 13 months. Many parents are understandably worried about the effects of so many vaccines on their child’s developing immune system – concerns that were hardly allayed by Dr Paul Offit’s assertion that, “Each infant would have the theoretical capacity to respond to about 10,000 vaccines at any one time”. Given Dr Offit’s financial interests, their reaction is perfectly logical.
We could not find any clinical trials looking directly at health consequences on children of the full schedule of vaccinations, in any country. Before a vaccine is used, it undergoes clinical testing, but this is done solely on the particular vaccine in question, by the vaccine manufacturer. Many argue that such testing is thoroughly inadequate and not sufficiently transparent. Once the vaccine is in use, monitoring continues, this kind of surveillance being regarded as one of the most important phases of vaccine safety monitoring. The problem is, as we've seen with work on the MMR/autism association, the difficulty in associating cause and effect in such retrospective, observational research, becomes a major challenge (one that the vacine manufacturers are able to exploit for profit). Vaccination awareness groups in the USA point out that many chronic diseases and disability have become far more prevalent as the complexity of the childhood vaccination schedule has increased.
This might be because of the view prevalent among health authorities and many researchers that it is unethical to compare vaccinated with unvaccinated children, since not vaccinating risks exposing the subjects to diseases they would not catch if vaccinated! By assuming that vaccines are effective, such circular logic pre-empts the outcome of clinical trials and prevents the proper research from being performed. Recently, a German group has begun utilising a questionnaire-based approach to examine the health of vaccinated and unvaccinated children, but this is hardly adequate. What’s required are prospective, randomised comparisons of children who undergo the full vaccination schedules with children who are not vaccinated at all – but we aren’t holding our breaths for those trials to kick off.
5. The human papillomavirus (HPV) vaccine for cervical cancer is being pushed hard on adolescent girls. Obviously cervical cancer is a terrible disease – are there any risks from the vaccine and will it fully protect girls who receive it?
We aren’t going to beat around the bush with this one: the HPV vaccine is ‘modern snake oil’. In fact, it’s much worse, because not only is it largely ineffective and founded on incomplete science, but it is also associated with a long list of side effects up to and including death. To top off this unattractive package, the vaccine is the subject of astonishing media deceit. We cannot find any real evidence that this vaccine is effective for girls of any age and now this pharma cash-cow is being proposed for boys to, supposedly, “…tackle the spread of the virus”. And now we’ll tell you why this is so scary.
The theory behind the HPV vaccine is that preventing infection with HPV will protect girls and women against cervical cancer, since the virus is known to cause the condition. However convenient the theory, there are a several problems with the practice of HPV vaccination as it currently exists:
- The vaccine protects against a maximum of two HPV strains, of which there are 15
- All we know for sure about the vaccines are that they produce a strong immune (antibody) response against the relevant HPV strains. Whether this translates into protection against cervical cancer is entirely unknown
- Clinical trials of HPV vaccines were performed in girls and women aged 16–23, yet they are being given to girls aged 9 years and above
- The HPV vaccines are the first genetically modified vaccines
- Vaccinating against HPV ignores other important risk factors for cervical cancer
- The HPV vaccine is associated with numerous serious side effects, and has so far been linked with 71 deaths – and this is according to the US Centers for Disease Control and prevention (CDC)
Despite all these problems, however, the US media have been falling over themselves to paint the HPV vaccine as the best – and safest – thing since sliced bread. The worrying result is that 12-year-old girls in California can now get the HPV vaccination entirely without their parents’ knowledge. We can expect a similar attitude in the UK: news that health authorities are switching from GSK’s Cervarix to Merck’s Gardasil – the one associated with 71 deaths, remember – was greeted with fawning adulation.
We are all for vaccine choice, but in this case, a combination of unknown efficacy, poor science, dangerous side effects and media lies makes the HPV vaccine one to avoid. We just hope that it doesn’t become mandatory, anywhere, any time soon.
6. As winter rolls around, there’s a strong push for people to receive the flu jab. This is even more the case since the swine flu outbreak of 2009. What’s the evidence for and against?
Pro-vaccination campaigns from various quarters are noisier than ever this year, whether from governments and national health bodies, local health authorities, pharmacies, drug companies and even supermarkets.

A UK supermarket now offering flu jabs in its in-store pharmacy....
....and tempting shoppers with a free coffee!
The swine flu ‘pandemic’ of 2009 appears to have been massively hyped up in order to makes lots of lovely money for the pharmaceutical companies, with World Health Organization officials in the pocket of Big Pharma. Interestingly, however, while there is absolutely no suggestion of a 2011 influenza ‘pandemic’, campaigns urging people to queue up for flu jabs are just as prevalent – if not more so.
Right at the outset, flu vaccination cannot offer complete protection from the virus, for a very simple reason: there are many different viruses that cause influenza, and new mutations appear regularly. Each year, medical committees advising health authorities meet to sit down, look at the evidence and decide which flu strains are likely to be most prevalent in winter; the yearly flu vaccine is then made up to protect against these top strains. This year, for example, the UK is vaccinating against influenza A (H1N1) pdm09 and H3N2 and influenza B. If that sounds a bit like someone sticking their finger in the air to work out which way the wind’s blowing – it is. If the ‘great and the good’ get it wrong and a different strain becomes prevalent that year, the vaccine won’t work.
But how deadly is influenza? In 2005, the most recent year for which figures are available, the US CDC reveals that only 1,806 people died from influenza. Far more people – 60,998 – died from pneumonia, a bacterial disease that is often the cause of death among the elderly, the sick and people with weakened immune systems who catch the flu. Studies have shown that vaccinating against flu does not protect the elderly or middle aged from contracting pneumonia.
As for vaccine effectiveness, the well-respected Cochrane Database has concluded that vaccines prevent influenza in children aged above 2 years, but that there is no evidence of a protective effect in younger children. A separate analysis of the Cochrane Database decided that flu vaccines are protective in adults aged 16–65 years and children aged 6 years and over, but results in other groups were inconclusive. Yet another Cochrane analysis found little ‘real-world’ effects of flu vaccination at all, and Simonsen et al found that many studies vastly overestimate vaccination benefit. Recommendations from health authorities go well beyond this, however. Anyone considering taking a flu vaccine should also consider the other substances present in the vaccines and the possibility of side effects.
Whatever the truth, influenza itself and flu vaccination aren’t going to disappear as issues anytime soon, especially with a ‘universal’ flu vaccine around the corner – although we are highly sceptical that it will ever materialise! With news that one scientist with a malfunctioning moral code has mutated the H1N1 bird flu strain into something far more deadly, we must all be on our guard – but we question whether vaccination is the answer.
7. With so much emphasis on vaccinations to protect our bodies from infectious diseases, mainstream medics seem to forget the vital role of our immune system. Can our immune system protect us from all diseases and what can we do to help it to function as effectively as possible?
We’ve said it before and we’ll say it again: the human body is a miracle, and nothing more so than the immune system. Looked after correctly and in optimum health, our innate and adaptive immunity should deal with pretty much anything it encounters. The best way to support your immune system? Eat a fresh, healthy and varied diet that’s organic as far as possible, is higher in protein and healthy fats and lower in starchy carbohydrates and dairy, don’t smoke, drink to excess or take recreational drugs, get sufficient exercise, get plenty of high-quality sleep...all the common-sense things that everyone who wants to avoid chronic disease should be doing!
In addition, there are several specific nutritional strategies for natural immune-system support. In a report written in 2006 at the request of the World Health Organization, ANH-Intl highlighted the enormous amount of scientific evidence in support of the following:
- Zinc
- Vitamin C
- Vitamin B12
- Vitamin A (and retinoids)
- Silver
- Other micronutrients, including omega-3 oils and vitamin E
- Beta-glucans
- Resveratrol
- Garlic
- Black elderberry
- Echinacea
- Other natural products, including curcumin and cat’s claw
And all of this was before vitamin D was hailed as one of the master controllers of the human immune system.
In the event of a pandemic, natural approaches such as these have several intrinsic advantages over pharmaceutical methods such as vaccines:
- Easier to rapidly accelerate production
- Lack of side effects
- Small chance of viral or bacterial resistance to nutrients
- Low cost
- Easy for the public to self-administer
- Public reassurance that nutrients are easily available, thereby reducing stress and panic
- Reduced burden on services, such as community doctors and hospitals
Allow us to end with a quote from that report: “In the event of a severe influenza pandemic, nutrient-based therapies administered worldwide would dramatically reduce mortality and morbidity and the dismissal of such therapies by global and national health authorities would result in the unnecessary loss of tens of millions of lives. We believe that such a dismissal would come to be seen as one of the greatest acts of professional negligence in human history.”
[1] Miller NZ. The polio vaccine: a critical assessment of its arcane history, efficacy, and long-term health-related consequences. Medical Veritas 2004;1:239–51.
[2] Englehardt SJ, et al. Measles mortality in the United States 1971–1975. Am J Public Health 1980;70:1166–9.
[3] Offitt PA et al. Addressing parents' concerns: do multiple vaccines overwhelm or weaken the infant's immune system? Pediatrics 2002;109:124–9.
ANH Vaccine Choice campaign page








Comments
your voice counts
02 December 2011 at 8:43 pm
This topic is probably one of the most difficult to discuss openly and freely. Every parent has to decide what they need to do to protect their children, probably the most basic of human instincts. There is such a lot of emotional investment involved whether you are for or against vaccination.
My wife and I decided against vaccinations in general, but recognise that it is by no means a cut and dried issue. Wish it were!
The wisdom gained from the evolutionary process should be recognised. We are so short sighted as a society, we really need to be more respectful of our origins as a species amongst others.
RCT's are the best way to measure scientifically any social experiment-though they are by no means infallible. Big Pharma would never attempt to use the conventional model to test the hypothesis that vaccination is truly safe for all children and will benefit every individual's innate immunity. It'll never happen.... they could never risk the financial consequences of failure.
07 December 2011 at 12:14 pm
You have stated that Gary Null PhD had a wide-ranging look at the literature on vaccination in general, and came to a startling conclusion: “Of thousands of articles in the peer-reviewed literature on immunology nowhere can we find gold standard, double blind, placebo controlled studies that prove that any vaccine or combination of vaccines can be shown to provide lifelong immunity and safety to any individual.”
So I have gone and looked at that original article published on Gary Null’s website (it appears you have based your Q&A on it) and there is no mentioning of any kind of how many articles or studies he has looked at. In the bibliography at the bottom of his article are listed 25 sources. So lets look at what are they: National Public Radio; Alternatives Medicine Digest, JeffersonT, Physical Interventions to Interrupt or Reduce the Spread of Respiratory Viruses, Clinical Diseases, Naturallnews.com; Washington post to mention some which are not by any means studies or source of reliable information on the topic. There are only 6 sources that may be studies related to the topic. There is no mentioning on even one study published in any recognizable Medical journal. So out of the hundred studies that are out there he has picked the handful that suit his thesis and completely ignored the overwhelming rest which actually support the case for vaccination.
If Garry Null was genuinely interested if vaccination is working he could have done a proper study. With setting a specific hypothesis about what he wants to find out lets say vaccination and consecutive cases or outbreaks in measles. Then he can set up himself to look at all studies he can find (information on them is readily available) in the USA since 1950 till 2011 for example. Then he can present us with comparison between the studies he has researched and how many of them support or are against his hypothesis. Instead he has presented us with a mash of ideas which are poorly supported using some scientific language and trowing some graphs to make things look believable. That is to say least very pour of someone ho puts PhD behind his name
And now let look who Gary Null is himself? He claims to be PhD but no where in his website is mentioned where is his PhD from. Nor there are any publications or research he has done in the area of immunology or epidemiology to show us that he is an expert in this area. In his website he has links and articles about Banking, Barak Obama, Wall Street, Iraq…!? to mention some. He also has a shopping page where supplements, oils and other paraphernalia can be purchased if you have a credit card. Can you imagine any GP or medical doctor to set up website and start endorsing brands or medications for his clients to buy if they wish so!? If this happens this doctor will be lynched by the media, ostracised by his pears and struck of the medical board for professional misconduct. However there is no issue for Dr Gull in doing that!? He has a financial interest in people purchasing his potions so he can make more money and he can do and say whatever fits his agenda as long as the orders are coming!!
In conclusion Gary Null seams to be one of those small scale operators scamming of people’s fear and illnesses. Exactly what big pharma has been doing just in a smaller scale. If Adam Smith your Science and Communications Officer, ANH-Intl would like to know how to spot a bad study he can read Bed science by Ben Goldacre. Where he can learn how the big companies are fixing their studies and how small fish like Dr Null are fuelling the supplements industry.
09 December 2011 at 1:44 pm
Dear Maryana
Many thanks for your comment. And many thanks for the compliment! Since you have taken issue with only two paragraphs of a 3500-word article, we can only assume that you approve of the rest. So thanks very much for your support!
On the other hand, you may be cherry-picking – that is, choosing a tiny part of the overall article in isolation – in order to make your point. In this case, the ‘tiny part’ of our article that you don’t like consists of a single link to a single article on Gary Null’s website, in a piece that includes a large number of references on a variety of vaccine-related topics. Far from basing our entire Q&A on it, as you suggest, we used Dr Null’s article to illustrate one point in a single question – i.e. that vaccination does not equal immunisation.
We could just as easily have pointed to Dr Andrew Wakefield’s 250-page report on the safety of the measles, mumps and rubella (MMR) vaccine that led him to recommend single vaccines instead – but that one’s not easily available, and we doubt that you’d appreciate being pointed to Dr Wakefield any more than to Dr Null. We could have steered you toward books by Viera Scheibner [http://www.vierascheibner.com/index.php?option=com_content&view=article&id=52:vaccination-by-viera-scheibner&catid=64:vaccination-book-by-viera], Dr Robert Mendelsohn [http://www.amazon.co.uk/Confessions-Medical-Heretic-Robert-Mendelsohn/dp/0809241315/ref=sr_1_3?ie=UTF8&qid=1323358801&sr=8-3], Dr Richard Halvorsen [http://www.thisislondon.co.uk/news/article-23404585-are-vaccines-a-waste-of-time.do] and a host of others. But instead, we’ll issue you a challenge: can you find, in Dr Null’s words, “Gold standard, double blind, placebo controlled studies that prove that any vaccine or combination of vaccines can be shown to provide lifelong immunity and safety to any individual”?
You have, for some reason, misrepresented Dr Null’s article. Rather than being bereft of, “Even one study published in any recognizable Medical journal”, it references articles from the New England Journal of Medicine, Vaccine, the British Medical Journal (twice), the Journal of Immunology and Occupational Medicine. The other references are perfectly mainstream and respectable, such as the US Department of Health and Social Services, Reuters and the Washington Post. Since his article is not meant as an officially published review article, Dr Null is under no obligation to list every single study that he reviewed to come to his conclusion – although we agree it would have been useful had he done so.
You also question Dr Null’s credibility. He has appeared before US Senate hearings into vaccination [http://www.youtube.com/watch?v=LYZBjZH1t0w&feature=related], so we assume he knows his stuff. It is neither here nor there whether he sells products on his website – everyone has the right to make a living. As for his qualifications, Wikipedia states that Null obtained his PhD via a distance-learning course [http://en.wikipedia.org/wiki/Gary_Null]. The fact that Dr Null was an 'external' student does not in itself suggest that his qualification is anything other than valid. And we fail to see why having an opinion on current affairs disqualifies him from researching vaccination!
Finally, we hope you won’t be offended if we don’t take you up on your recommendation of Ben Goldacre’s book. The man is not what he proclaims to be [http://www.slingshotpublications.com/dwarfs.html], and ‘Bad Science’ is exactly that – a collection of appallingly bad science, misrepresentations and half-truths. We would go further, and caution you against using his model of ‘science’ as any kind of guide to life: you may well end up looking rather silly.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences