A comprehensive new report paints an alarming picture of the threat to human health and fertility posed by human-made endocrine disruptors. As artificial fertilisation techniques are offered to increasingly older women, will they deliver the intended reward or are such solutions doomed to fail without a broader view of the infertility jigsaw puzzle?
WHO’s second look
The idea that human-made chemicals in our environment may be having profound effects on human health and ecosystems is nothing new. Indeed, the first World Health Organization (WHO) report on the vast array of industrially-produced chemicals known to disrupt hormonal (endocrine) systems in animals including humans was published in 2002. Back then, the science was sparse and the report concluded that the overall data linking endocrine-disrupting chemicals (EDCs) and human health effects were “weak.”
Now, in 2013, far more scientific evidence is available – leading to much more sobering conclusions on the part of the WHO.

State of the science: sobering yet incomplete
Among the findings of the WHO’s new report, State of the Science of Endocrine Disrupting Chemicals are the following:
- “Human and wildlife health depends on the ability to reproduce and develop normally. This is not possible without a healthy endocrine system” – an inevitable conclusion, bearing in mind the enormous complexity and infinitely precise balancing of the endocrine system
- EDCs are now almost ubiquitous worldwide
- Up to 40% of young men in some countries have low semen quality, and the incidence of genital malformations, including undescended testes (cryptorchidism) and penile malformations, in baby boys has either increased over time or plateaued at high levels
- Adverse pregnancy outcomes, such as preterm birth and low birth weight, are on the rise in many countries
- Nearly 800 chemicals with known or potential endocrine-disrupting properties have been identified – yet only a tiny fraction have been specifically tested for these effects in intact organisms
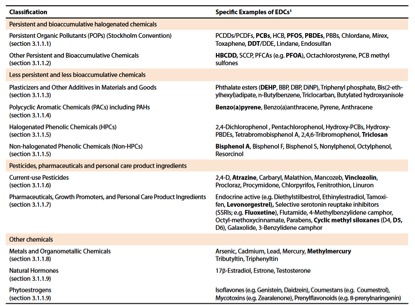
- Known ECDs (Table 1) include diethylstilboestrol (DES), polybrominated diphenyl ethers (PBDEs), benzopyrene, bisphenol A, lead, arsenic, cadmium and methylmercury
- Organisms are most sensitive to EDC exposure during critical periods of development, such as foetal maturation and puberty
- Authorities and healthcare systems worldwide have overlooked or ignored the environmental contribution to the rising incidences of endocrine disorders
- The test methods that have been agreed and validated for the purpose of identifying EDCs regularly overlook important effects – and, “Disease risk due to EDCs may be significantly underestimated”
UK health service recognises rising infertility rates
In the same week that the WHO report was released, the UK’s National Institute for Clinical Excellence (NICE) announced that it would extend funding for in-vitro fertilisation (IVF) to women aged 40–42 years, up from the previous limit of 39 years. In doing so, NICE recognised [http://publications.nice.org.uk/fertility-cg156] that, “Infertility affects 1 in 7 heterosexual couples in the UK. Since...2004 there has been a small increase in the prevalence of fertility problems”. As Figure 1 shows, most of the increase in UK fertility problems is due to ‘unexplained’ and male factors.
The question must be asked: could the rising incidence of infertility be at least partially related to environmental endocrine disruptors of the type described in the WHO report? In men, the limited evidence available suggests links between certain EDCs and reduced sperm quality; and while plausible biochemical mechanisms exist for the role of EDCs in female infertility, the report itself notes that, “There is...almost no evidence for causation of...infertility [by ECDs]; however, few studies have examined chemical causation of these diseases directly, and very few chemicals have been investigated”.
This is, of course, code for there being a data gap the size of the Grand Canyon, and absence of evidence is not evidence of absence – despite what the chemical lovers at Sense About Science and elsewhere would have us believe.
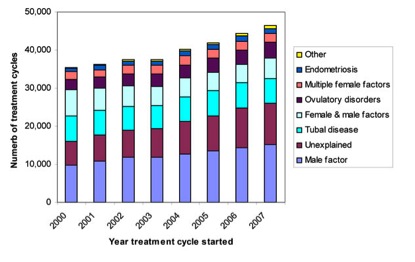
Figure 1. Types of infertility treated in the UK by IVF and ICSI treatment, cycles started 2000 to 2007. Taken from the UK Human Fertilisation and Embryology Authority website
Something’s not right here
On the basis of what is already known about the insidious low-dose effects and wide distribution of EDCs, we’d frankly be amazed if EDCs weren’t implicated to some degree in the rising rates of both female and male infertility.
But we have to wonder whether making IVF ever more available is the right way to address the infertility epidemic. Quite aside from its traumatic, prolonged and often unsuccessful nature, IVF treatment involves a big whack of artificial hormones – which, going by the WHO report and the history of hormone replacement therapy, may aid conception in the short term but cause untold problems in the future. Not least of which is adding further EDCs to municipal drinking water supplies, waste and natural water courses.
And, of course, apart from hormone-related mechanisms, infertility may be associated with a host of diet and lifestyle factors: insufficient or excessive exercise, heavy metal contamination, stress, lack of sleep, micronutrient deficiencies and electromagnetic pollution, to name some of the most prevalent. A programme designed to give the body a ‘spring clean’, while building it up with a clean, nutrient-rich diet possibly assisted by targeted food supplements, seems the most logical way to boost fertility – but here, in the UK, NICE and the NHS have virtually nothing to say.
WHO has put EDCs on the international radar
We hope that the WHO report will prompt governments and health authorities to spend taxpayers’ money on thoroughly investigating the links between endocrine disruptors and health and fertility effects. In the meantime, the precautionary principle should be used to encourage much tighter controls of industrial and pharmaceutical chemicals and waste.
In the meantime, those interested in natural methods of fertility enhancement should do their due diligence. Our friends at the UK charity Foresight Preconception have for many years helped thousands to become pregnant. Similar organisations exist in other parts of Europe and around the world.








Comments
your voice counts
03 March 2013 at 9:55 pm
Great article.
I know you are very much on-board already with the dangers of wireless radiation/EMR already, but non-ionising electromagnetic radiation (wifi, cell phones, etc) has been shown to cause endochrine disruption also - so we have to worry and alert people to not just chemicals/EDCs but also EDFs - Endochrine Disruption Fields!
The following studies (from a quick search so there are likely many more) showed ED from EM fields (listed here in order of Symptoms, Title of the study, Authors, Date and Type)
Variations of Melatonin and Stress Hormones "Variations of melatonin and stress hormones under extended shifts and radiofrequency electromagnetic radiation" Vangelova KK, Israel MS 2005 Human
Thyroid Dysfunctions "Are thyroid dysfunctions related to stress or microwave exposure (900 MHz)?" Bergamaschi A, Magrini A, Ales G, Coppetta L, Somma G. 2004 Human
Pituitary Cortical Adrenal System "Experiments on the relation between shortwave irradiation and the pituitary cortical adrenal system” (M1)" ADLER, E., & MAGORA, A. 1955 Human
Nerve Growth Factor/Phenochromocytoma Cells "Exposure of nerve growth factor-treated PC12 rat pheochromocytoma cells to a modulated radiofrequency field at 836.55 MHz: effects on c-jun and c-fos expression" Ivaschuk OI, Jones RA, Ishida-Jones T, Haggren W, Adey WR, Phillips JL 1997 In Vitro
Nerve Growth Factor/Phenochromocytoma Cells "Exposure of nerve growth factor treated PC12 rat phenochromocytoma cells to a modulated RF field at 836.55 MHz" Ivaschuk OI, Ishida-Jones T, Adey WR, Phillips JL 1997 In Vivo
Excretion Rates of Stress Hormones "The effect of low level radiofrequency electromagnetic radiation on the excretion rates of stress hormones in operators during 24-hour shifts" Vangelova K, Israel M, Mihaylov S 2002 Human
Adrenal Cortex "The functional condition of the adrenal cortex in ship specialists who are subjected to the action of a super-high frequency EM field" AFANAS’YEV, B. G. 1968 In Vivo
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences