Content Sections
By Meleni Aldridge, Executive Coordinator, Director ANH-Intl
This article aims to be part evolutionary history lesson and part life-changing, health-enhancing, impactful information, which also pretty much reflects the rapidly emerging discipline of clinical psychoneuroimmunology (CPNI), the therapeutic discipline of my postgraduate study. I make no secret of the fact that were it not for my CPNI studies, I don’t think I would be enjoying the level of physical health and vitality I have now, or been able to claw my way back fully from autoimmune thyroid disease. It's quite literally been pivotal in my healing — and for many others too. If it were down to me, I’d make CPNI the foundation of any nutritional, naturopathic or integrative medicine course.
You can read more about CPNI at the end of this article and how you can explore further with a masterclass we are hosting later this week on Friday 17th November with the founder, Dr Leo Pruimboom. But right now, let’s talk a bit about a stealth metabolite that masquerades as a harmless, inert, waste product — that just isn’t.
Uric acid - stealth metabolite
As Dr David Perlmutter says in his 2021 book, Drop Acid, uric acid (UA) is cast as a trivial, incidental by-product of normal biology, excreted in urine, and to a much lesser extent, in stool, that’s relevant only to those who have suffered from gout or kidney stones. Despite much of conventional medicine looking at UA only in these terms, it’s actually a key metabolite involved in just about all regulatory mechanisms that sits at the centre of our most fundamental metabolic processes. The kind of processes that make our bodies run like the intricately complex, well-oiled, evolutionary-robust beings we were designed to be. Then we modernised life…

But what exactly is uric acid?
It’s a metabolite that occurs naturally in the body as a result of the breakdown of purines, which are nitrogen-containing compounds that are found in DNA and RNA, that can be found in higher amounts in certain foods and tissues (exogenous sources), and are produced also in the body (endogenous sources) given their vital role, along with closely related pyrimidines, as building blocks of all new cells.
It’s usual to see uric acid measured on standard blood tests because it’s a helpful marker indicating the level of acidity in the body. However, the standard reference range is fairly broad, and it’s mostly overlooked until someone is showing symptoms in either their joints or kidneys.
As a metabolite of purines, the body will always excrete a level of UA in urine, but elevated levels are more often seen as just a marker and causative agent of gout and in the longer term, kidney stones. We now know that when levels exceed those at the lower end of the conventional medical reference range (under 300 μmol/L in the UK, or 5.5 mg/dL in the US), a myriad of downstream health issues can ensue. Health issues like obesity, insulin resistance, type 2 diabetes, high blood pressure, coronary heart disease, non-alcoholic fatty liver disease, stroke, neurological diseases (dementia, Alzheimer’s), cancer and premature death.
The reality is that our biggest killers in the developed, modern world, have UA at their heart, leaving gout and kidney stones very much as the lesser of its evils. You see now why I call it a stealth metabolite. It’s anything but an innocent waste product. Although UA has been described for centuries — even as far back as 1200 CE (BC) in the description of a condition called podagra — medicine hasn’t sufficiently connected the dots between hyperuricemia (high uric acid levels) and the vast range of chronic diseases many are suffering.
Podagra was essentially what we know today as gout, but it’s an indication that the health practitioners of yesteryear recognised UA as a problem, earning its historical label, a ‘rich man’s disease’, because of its link with meat and alcohol. It was always thought of as a disease of overindulgence. Today, whilst it's conventionally acknowledged that some people are more susceptible to gout or kidney stones than others, what we really need is more awareness and tracking of UA levels in the body on a very regular basis. If we keep UA within the body’s natural management capacity (ideally under 300 μmol/L in the UK or 5.5 mg/dL in the US), we could prevent many from beginning the descent into chronic disease and neurodegeneration long before the body shows any symptoms of dysfunction.
Sources of uric acid
Excessive levels of circulating UA result from the consumption of purine-rich diets, the body then produces excessive UA as a by-product of purine metabolism, and can't always excrete it fast enough in the urine.
Foods that are rich in purines contribute specifically to the body's UA production. These include animal protein (particularly game), organ meats, seafood, fish (anchovies, herring, mackerel, sardines, tuna, trout are some of the highest), alcohol, and — wait for it — fructose, especially high-fructose corn syrup. Some alcohol, like beer, contains purines, but in the main, alcohol increases the metabolism of purines that are then metabolised to UA, as well as increasing the lactic acid levels in the blood. Alcohol also affects the way the kidneys process waste products, which in turn affects how UA is eliminated in urine. It’s as if alcohol causes UA to be sucked back into the body again where it can build up to form the characteristic, gout-associated crystals in the joints, increase inflammation and generally wreak its stealthy havoc through our metabolic pathways. As we approach the festive season, this isn’t the most jolly news, I know, but if it’s any consolation, wine seems to be the better choice over beer and spirits — in moderation of course and only if you’re not already suffering hyperuricemia!
it's important to know that UA is also generated as a by-product of fructose metabolism, so sugar, which is 50% glucose and 50% fructose, and high fructose corn syrup (and similar cheap sugars added to processed foods) are huge contributors. Whilst there are certain purine-rich vegetables like spinach, mushrooms and asparagus, they don’t contribute to a rise in UA like high fructose containing foods and beverages.
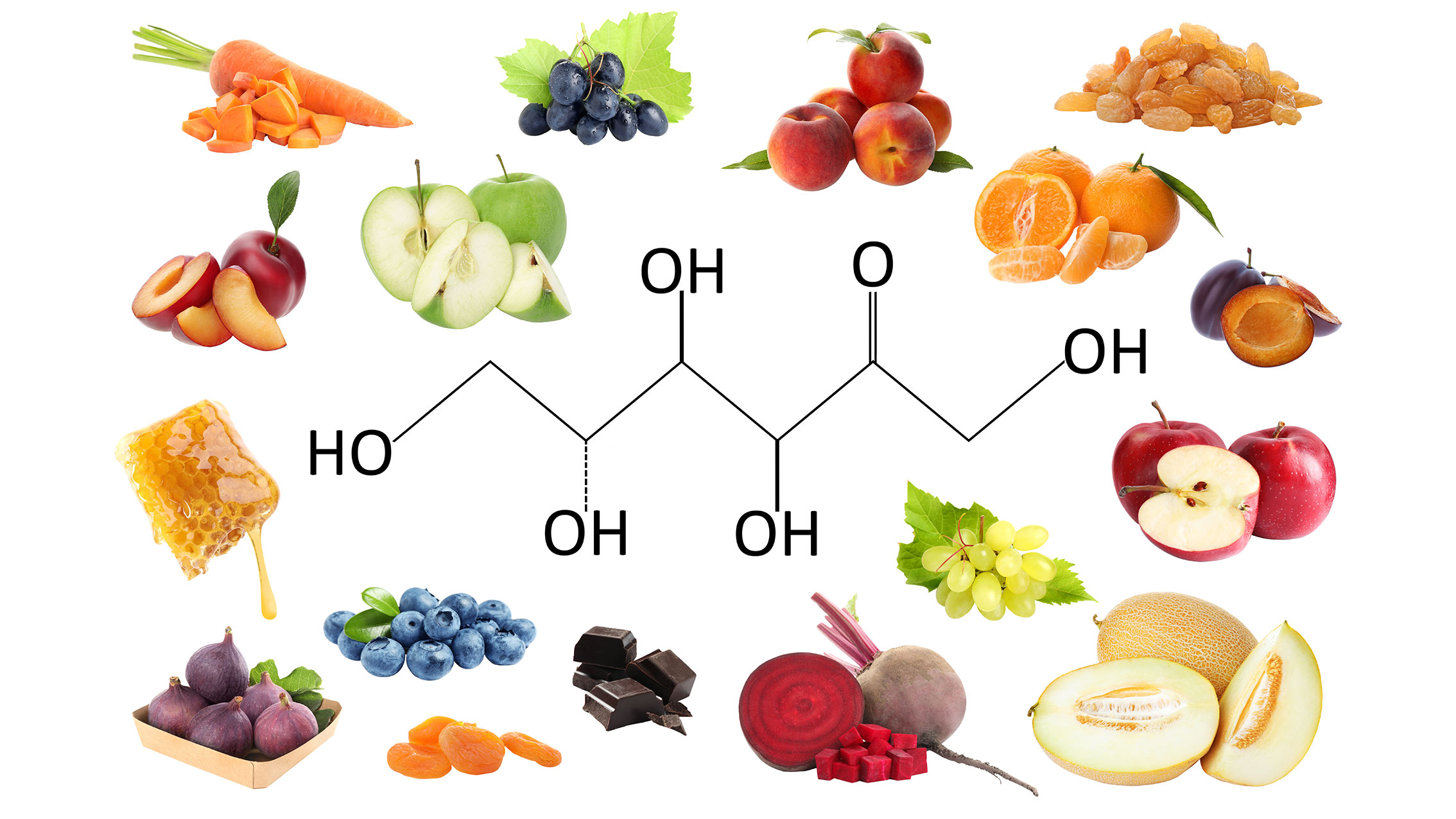
We also make UA naturally as a by-product of metabolism and the breakdown of purines in the body. Under normal circumstances the kidneys filter out UA and it’s excreted in our urine with a little in the stool. But when UA levels exceed what the kidneys can cope with, we now know it’s wreaking havoc, stealthily, without any symptoms. Not everyone shows hyperuricemia through gout or kidney stones, which occur when UA builds up and forms crystals that settle in the joints (most often the big toe) or the kidneys. Both are extremely painful conditions, but not as life threatening as the host of other chronic diseases it causes, or degeneration of the brain and nervous system.
The uricase mutation - survival trade off?
Our journey through evolution is littered with genetic mutations, trade-offs if you will, to ensure our survival as the environment around us changed. Hence, mutations are all about risk and benefit. You gain something that is linked to ensuring survival, but in the process you may heighten the risk of something else that may be unpleasant, but not life-threatening. The disconnect between our genome, established a couple of hundred thousand years ago, and our environment now is what we need to understand given the evolutionary/environmental mismatch. To bring this to life more - it takes between 40,000 to 70,000 years for us to make significant changes to our genome, particularly of the kind that would allow our bodies to cope with many of the 'foods' of today.
The uricase mutation is one such mutation — mismatch — and represents a fascinating aspect of our human genetics that has had a significant impact on uric acid metabolism. Uricase, also known as urate oxidase, is the enzyme responsible for breaking down uric acid into a more soluble compound, allantoin, to facilitate its excretion. However, some species, including primates and us, humans, have undergone evolutionary changes (mutations) which have resulted in the loss of functional uricase during the Miocene epoch. This loss is attributed to a mutation in the gene responsible for encoding uricase (URIC1) and means that we now can’t break it down in our bodies to a more soluble form, but have to excrete it as UA.

(You won't be surprised to find that the above are very definitely not on a low purine/uric acid diet!)
While the uricase mutation might seem like a disadvantage due to associated health risks, the prime hypotheses are that it occurred in response to the prior mutation in vitamin C synthesis, which increased our levels of oxidative stress. Higher UA may have played a role in protecting early humans from oxidative stress, positively impacting ageing and cancer. Also, that the loss of uricase activity allowed our ancestors to readily accumulate fat via the metabolism of fructose from fruits, which would have been a huge benefit with the loss of access to energy-rich rainforests, combined with seasonal climate change in Europe, at the end of the Oligocene epoch. This increase in UA also increased blood pressure, helping us to endure periods of dehydration and lack of salt.
We have been very deliberately genetically programmed to create fat from fructose with ease. Survival of the fattest! It’s no wonder that there is such a clear correlation between the rise of high fructose corn syrup and sugar in general, with a downturn in population health and the exponential rise in obesity and chronic disease.
Ten keys to lowering your UA level - and keeping it there!
- Invest in a uric acid home testing kit. Blood spot is the most accurate and there are many inexpensive ones on the market. Some give you a 3-in-1 reading with blood glucose, cholesterol and uric acid. You can also get ones that measure ketones as well as uric acid. Whichever you get, home monitoring and knowing your numbers is key.
- Adopt a diet that’s low in purine-rich foods 80% of the time. Incorporate more vegetables, fresh herbs and spices into your eating and make whole, unprocessed and organic (if possible) foods a priority.
- Watch your consumption of fruit and remember that we’ve been designed for very low-sugar fruit, consumption, which is why berries are still best - and give you a whack of antioxidants too.
- Avoid processed foods that contain high fructose corn syrup (HFCS) or its relatives, eg. maize syrup, glucose syrup, glucose-fructose syrup, tapioca syrup, crystalline fructose or isoglucose.
- Get keto-adapted. You won’t be surprised to find out that a diet most closely related to our evolutionary-norm, such as the eating guidelines we outline in our Food4Health campaign or our book, RESET EATING, combined with intermittent fasting, is also a very healthy lowering UA diet too.
- Stay well hydrated and support your kidneys with flushing out excess uric acid with plenty of fluoride-free, ideally chlorine-free, clean water. If you can structure your water before you drink it, then so much the better.
- Manage your weight. Obesity is a risk factor for elevated uric acid levels, as well as increased inflammation, which predisposes you to dysfunction and disease.
- Reduce your alcohol consumption. Especially of beer and spirits to help manage UA levels. But remember alcohol is a toxin and reducing consumption will also lift a burden off your liver and your entire detoxification system - your microbiome will be forever grateful too and return the favour in spade loads.
- Do get active regularly. Being repeatedly reminded to exercise may get very boring, but we have been made to engage gravity daily, multiple times a day. It not only gets you fit, keeps your muscles and joints moving and wards off disease, but it also helps lower UA levels.
- Employ the support of UA lowering supplements. Dr Perlmutter’s top 5 are quercetin 500 mg, luteolin 100 mg, DHA 1,000 mg, vitamin C 500 mg and chlorella 1,200 mg per day, but there are others. Please also remember that it should always be food first - then some targeted supplementation if further support is needed. Supplements are not, and should never be seen, as magic bullets!
I find our evolutionary history fascinating, and for me, the insights into the ‘why’ of how our pathways work the way they do, helps my compliance with the nutrition and lifestyle choices that I know are going to net me the highest health return. The uricase mutation provides another captivating glimpse into the intricacies of human evolution and the delicate balance between genetic adaptations and health outcomes. While it creates an increased risk of high UA (hyperuricemia), we also now know exactly what to do to support our bodies in maintaining a low, healthy level. Knowledge is power after all. Understanding the impact of the uricase mutation not only enriches our knowledge of human biology, but also opens doors to more comprehensive self-empowered care.
If your interest has been peaked by evolutionary biology and its impact on our health…
There’s still time to make a spontaneous, possibly course-correcting, choice to join us for the clinical psychoneuroimmunology masterclass with Dr Leo Pruimboom, 'The case for drug-free medicine and 25 CPNI interventions', on Friday 17th November in London, or online.
Find out more about the event or to book
What is clinical psychoneuroimmunology?
Clinical psychoneuroimmunology (CPNI) is an exciting, rapidly evolving and translational field of medicine that explores the connections between the supersystem comprised of the mind, nervous, endocrine and immune systems. In the process, CPNI identifies clinical interventions that optimise multi-system function while positively influencing multiple risk factors known to activate disease mechanisms. It looks at how thoughts, feelings, and behaviours interact with our ancestry and epigenetic expression to create unique and individual traits that influence physical and psychological health — particularly immune function, which exerts influence on every cell in the body. It could more accurately be termed clinical psycho-neuro-socio-endo-metabolo-immunology.
CPNI is an ever-growing interdisciplinary science that is deepening our knowledge of how this communication network operates. Understanding the body's adaptive processes can help us identify relevant pathways for intervention to bring about positive change to health and wellbeing. CPNI is firmly rooted in evolutionary biology appreciating our genetic makeup and the environmental influences that shape the epigenetic expression of our genes.
>>> Buy your copy of RESET EATING by Rob Verkerk PhD, Meleni Aldridge and Melissa Smith
>>> Join as an ANH Pathfinder and immerse yourself in our supportive community - either as an individual, a health professional or a corporate member
>> Feel free to republish - just follow our Alliance for Natural Health International Re-publishing Guidelines
>>> Return to ANH International homepage









Comments
your voice counts
There are currently no comments on this post.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences