Content Sections
Dame Tessa Jowell’s death at the weekend from brain cancer has resulted in the UK government doubling its funding into research on brain cancer. It was also announced that the “gold standard dye” test (PET scan) would be rolled out nationally to help identify brain cancers sooner. Despite the ongoing investment into research, cancer rates remain stubbornly high, diagnostic tests are limited and can contribute to the development and spread of cancer and patients are offered limited treatment options.
Stacking the odds
In developed countries, cancer is the second highest cause of death. Current estimates are that 1 in 2 people are now at risk of developing the complex disease during their lifetime. Between 2006 and 2016 global cases of cancer rose 28%.
In the UK alone, it’s estimated the number of people living with cancer will virtually double by 2030. Look at most cancer statistics and they’ll tell you the increase is a result of us living longer, however according to Cancer Research UK the greatest increase in cancer rates since the early 1990’s is in the 0-24 age group.
Preventable risk
Many cancers are diet and lifestyle related and therefore preventable. Thirteen types are directly linked to obesity with alcohol consumption, smoking and diets high in processed foods and low in fruits and vegetables closely linked. So why isn’t more being done to prevent the development of cancer in the first place rather than most efforts going into the hunt for a drug-based miracle cure?
Receiving a cancer diagnosis is an overwhelming experience for most of us. As you struggle to come to terms with the news you’re often fast-tracked into a system of orthodox treatments over which you have little or no control, or have you? For many, scared by their diagnosis, they trust the path laid out by their oncologist, not knowing there are other, often safer, diagnostic and treatment options open to them. As knowledge grows, many cancer patients are now turning to non-standard treatments seeking a gentler, more natural way to beat their illness. They also recognise that these approaches help strengthen the body in ways that allow it to better handle both the treatments being given as well as supporting the body’s self-healing mechanisms.
What are your options?
Challenging the standard approach to cancer care will often meet with resistance and dismissal with many oncologists unwilling to engage in discussions about different diagnostic tools and therapies outside of the mainstream. Even the World Health Organization has recommended complementary medicines be integrated into national health systems, but we’re a long way from that happening yet in the UK and many other countries. Among the most progressive of integrative approaches is Ayurveda. These can be widely interpreted but in our view they should share at least the following 5 features. Integrative approaches to cancer care should:
- take fully into account the whole person and his or her internal and external environment (physical, nutritional, chemical, social, psycho-social, emotional, spiritual, etc)
- minimise the risk of spread of any malignant cells when seeking to diagnose or grade tumours (non-invasive or minimally invasive methods preferred),
- create an unfavourable micro-environment around tumours (e.g. ketogenic diets),
- use the most targeted treatment approaches that minimise any collateral damage to healthy tissues and cells, and,
- work to optimise the function of an optimised healing response (tumour suppression, immune system modulation, repair, etc.) in the body.
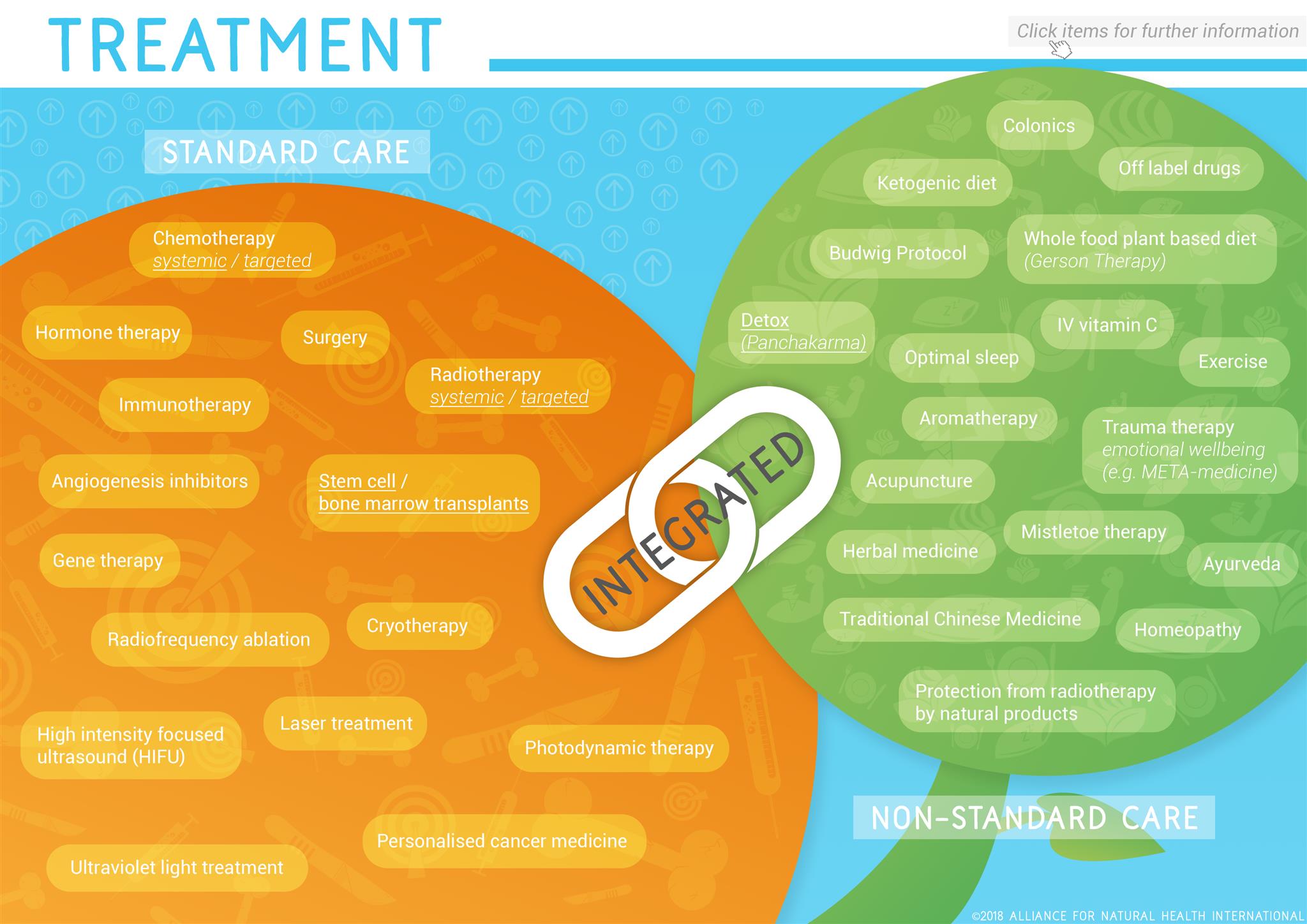
Asking the right questions, becoming empowered, doing your own research and seeking second, third or even fourth opinions is often the best way to prepare yourself for your journey. In an effort to make things a little easier, we’ve compiled an interactive infographic complete with links to further information that might be helpful to your process.









Comments
your voice counts
16 May 2018 at 10:30 pm
You will always find that as soon as you go against conventional methods of "healing cancers" you come up against many scientists / doctors who are so blinkered because they either don't want to know of "other cures" or are so in with the drug companies even to the fact that some are given back handers to sell the big pharma drugs ( which is of course a criminal act ) they dismiss any kind of "alternative / complimentary medicine". Also and even to the fact that there is proof from studies that certain healing methods do help and even cure in some cases but these are just dismissed again by the authorities as small fry and just don't want to know . Some doctors/oncologists are just beginning to see the light that the conventional way is not always the best and in some cases can make cancers worse than they were . It is up to us to let government health ministers know the facts of all these matters of concern and to believe that complimentary medicine has a greater role to play in healing in our modern world as many healing practices are far older than conventional they should all sit up and listen . PS , in your non-standard care notes I would also include Shiatsu therapy as there are many practitioners now working at hospices/NHS etc . I myself have also seen some recovering cancer patients in my practice and they have benefited much from Shiatsu as support for their ongoing recovery .
17 May 2018 at 12:02 pm
Thanks for taking the time to comment Paul and highlight the use of Shiatsu. It's always good to hear about additional therapies that we may not have considered.
Warm Regards
Melissa
17 May 2018 at 1:49 pm
And reflexology is useful and shows positive results in supporting and relaxing patients too.
24 May 2018 at 9:03 am
It is indeed a useful therapy to support patients. Thank you Karen
16 May 2018 at 10:51 pm
The cancer racket is so deeply disturbing that many will feel safer under conventional fears met by 'heroic interventions against the odds'. And that is a clue to the nature of the desire to be protected from greater fears by displacement narratives.
It is also an arena in which state power of law is used to deny and penalise open exploration and discussion. Only a lie seeks to defend from awareness and communication.
Of course the negative 'economy' is much more systemic than cancer, or pharma - being about the intent of control over life - and the power to check or manage the 'chaos' that arises from denied life.
It's the logical extension of a negative or fear defined sense of self-existence that gives power to the power to hide (protect from) fear.
17 May 2018 at 8:31 am
Having had cancer and standard treatment and invasive surgery I think it is so important to look after the mental and physical health ,particularly through the teens when young people more girls,but boys too are putting toxins on their skin and formulating ideas about alchohol. Food freedom for teenagers often means bad food, more young people now are suffering stress trying to compete in an unforgiving world. So whatever we can all do is positive
17 May 2018 at 10:43 am
Dear Chrissie, Thank you for taking the time to comment and yes positivity is one of the best forms of medicine.
With kind regards
Miranda
17 May 2018 at 10:10 am
I agree 100% with you and have always thought more money and effort should be put into prevention of Cancer than trying to find a "cure".
17 May 2018 at 10:45 am
Dear Isolde, thank you for commenting - one of the oldest sayings is "Prevention is so much better than cure"
With kind regards
Miranda
17 May 2018 at 11:15 am
There is a World Wide Cancer Fund which researches prevention strategies so I dontate to them rather than big pharma. They are a small outfit and very much under the radar but well worth supporting and making visible.
17 May 2018 at 11:58 am
Thanks for sharing Teresa.
Warm Regards
Melissa
19 May 2018 at 7:52 pm
I find it both interesting and sad that so many are resistant to the more natural, none Invasive Treatment options despite a growing evidence that nature knows best?
Even when I try sharing this type of information purely to raise awareness and to let people know that they do have other options the resistance is strartling!
20 May 2018 at 1:45 am
The fallacy: "Today's research, tomorrow's cure."
The truth: today's research, today's wages; tomorrow's research, tomorrow's wages.
And who is funding this fraud? We are, that is we the productive class, the tax paying people; we the forgotten people whose wealth is plundered in the form of gratuitous taxes; not by voluntary exchange, but by force of arms!
And are we ever asked how are money is to be spent? no never! Instead we are told!
And if we we have the audacity to question their rule, they will put a mirror in front of our face, telling us to talk to ours heart's content, and afterwards to go away, pay our taxes and stop complaining (questioning/challenging).
Friends, if ever we are told that we have cancer, or any other ailment, always seek sound medical advice. By that I mean turn your back on the so called doctor and go to those that truly know; those that really have your best interest at heart. Sites such as this are a wealth of information and good guidance.
26 May 2018 at 5:04 pm
I I have I am been told this.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences