Content Sections
We’ve been on a collision course for around 20,000 years. The crash occurred at the start of 2020 – and it’s still ongoing. The casualty in the crash is human resilience. The consequence is that a not particularly virulent and only moderately contagious virus has wrought havoc upon us. Building resilience in our populations and ensuring our countries are run by enlightened people capable of making smart decisions in this time of crisis would be a huge asset in our emergence from the wreckage.
But it appears most of us can no longer rely on governments to make smart decisions. Most are too deeply intertwined with the corporates whose products have contributed to our loss of resilience, whether it’s junk, low fat, refined carb-based foods, over-prescribed drugs or digital tech that’s turned us into couch potatoes.
So we’ve made a short video that gives you a whistle stop, crash course through our last 20,000 years of history, looking at key events that impacted our resilience as well as previous pandemics.
Our hunter gatherer ancestors, armed with the thrifty genotype that we still carry with us today, may not have had long lives. But on the whole they had bucket loads of resilience or at least plenty of opportunity to rebuild it following episodes of resilience-busting stress.
So please take a look at our new video – and SHARE, SHARE, SHARE. Please help us get the word out to others that building resilience is our key defence, not only against coronaviruses, but also to help us cope better with the ‘new normals’ that are being hashed out by governments that have the potential to cause untold damage to individual and societal health, rights and freedoms.
We’re told that science is driving government decisions, but how much is there to underpin what we’re being forced to do. Here’s a summary:
- Social distancing – conflicting science over benefits in many situations, no benefits in more confined indoor spaces with poor ventilation – widely mandated by governments.
- Lockdowns – conflicting evidence over benefits, causes serious damage to society and economies – widely mandated by governments.
- Mask wearing – conflicting science over benefits in most situations, may induce harms to users, may increase transmission through contact of damp masks – widely mandated by governments.
- Vaccines – no evidence yet the current candidate vaccines will be safe or effective – widely promoted by governments.
- Resilience – immune and psychological resilience are the only things that have been conclusively shown by science to protect us from immune challenges and stress – no or minimal guidance from governments!
>>> Find out more in ANH-Intl’s Covid Zone
Watch, learn and share
This is a true multi-media experience. If you've got a set of headphones please put them on to savour the full experience. Hold tight, your crash course takes just 5 minutes!
About the video
The majority of people in the world – it would seem – are gagging for a vaccine. A magic bullet – or injection – that we’re told could release us from the social and economic nightmare brought about by our response to a novel coronavirus, SARS-CoV-2. One enacted by governments, mostly with no recourse to public viewpoints or the democratic process. The public’s minds are being conditioned by sophisticated media messaging to expect that the liquid injected into their bloodstream will have the capacity to single-handedly rob the virus of any ability to cause harm to our bodies.
The reality is something different. If one or more of the current vaccine candidates ends up working, something that is as yet an unknown, it will be our immune systems that deliver the real goods – the antibodies that inactivate the virus. Contrary to what the public is often told, uncertainty over both efficacy and safety is high, especially given the most hurried development and evaluation of a vaccine the world has yet known. We’ll apparently get some data on safety from the earliest prototypes that are already in trials later this year, but assuming there’s enough of the virus still knocking about through this coming northern hemisphere winter, some data on the effectiveness against real world infection might be noisily fed into the public domain next year at the earliest. However slim the purported benefit as declared by a Gates Foundation and pharma-funded system that cannot be trusted to deliver transparent science, there will undoubtedly be people lining up regardless of the quality or certainty of the results, such is the power of the propaganda machine.
For a vaccine to ‘work’ – or for us to survive infection in the absence of an effective vaccine with nothing worse than mild disease – depends on how well our immune system functions when challenged by the real virus or a copy of a snippet from its spike protein. That’s a function of our immune system and general resilience. So what is resilience? It’s a term, first developed to describe psychological resilience; the ability of a person to bounce back from adversity, stress or trauma. It is now also used to look at other aspects of our function, not just our psychological responses. Therefore, we now can think about physiological resilience, and that will include our ability to respond to physical stress, chemical or EMF exposures, or even poor diets, eating patterns and habits. The stressor can take a multitude of different forms and may include our social or familial environments, including our inability to be nurtured by them if we’re isolated, our employment, or lack of it, and our financial status.
COVID-19: the multi-lateral stressor
The current Covid-19 pandemic opens up an array of new stressors that a study by the Mental Health Foundation suggests will generate an unprecedented array of mental health problems. The research community that has long existed in silos, is not well equipped to deal with the trans-disciplinary nature of the problem so is urgently calling on prioritisation of a new research approach for mental health science.
The pandemic has created something that’s so much more than a mere immune challenge. The human response to the virus, more than the direct effect of the virus itself, has decimated societies and economies. It has affected almost every aspect of human activity and recovery will inevitably take years. Some may face the consequences of what has happened in 2020 for the rest of their lives.
>>> Our articles remain free to access because of your generous donations
Close on half a million people have died with the virus so far. We don’t know how many deaths have been caused directly by the virus, although we do know that in the vast majority of cases severe disease and deaths are associated with comorbidities which reduce physiological resilience, in part because the immune response is less well modulated.
Only in retrospect will we be able to judge how appropriately or inappropriately we acted. We’re deeply concerned that, unless there’s a 180 degree turnaround sometime soon, the failure by governments and the mainstream medical community to address physiological resilience in the general population will one day be seen as one of the biggest failings of the Covid-19 pandemic era.
So here’s an important, potentially life-saving message: whatever you do, and whatever the universities and pharmaceutical companies dream up between them, focusing on developing resilience should be somewhere near the top of your list of health priorities for the coming year.
Yet we’re hearing virtually nothing in the way of public health advice in this area – from any government, anywhere in the world. Part of the reason for this is that the biomedical model is not set up to create health or resilience in the population. It is not proactive. Instead, it’s set up to treat or manage disease; it’s reactive (see Figure below). The need to create health throughout the lifespan of an individual – and to be able to do this outside the normal structures of the existing healthcare system, namely hospitals and clinics, is a central notion in our blueprint for health system sustainability.
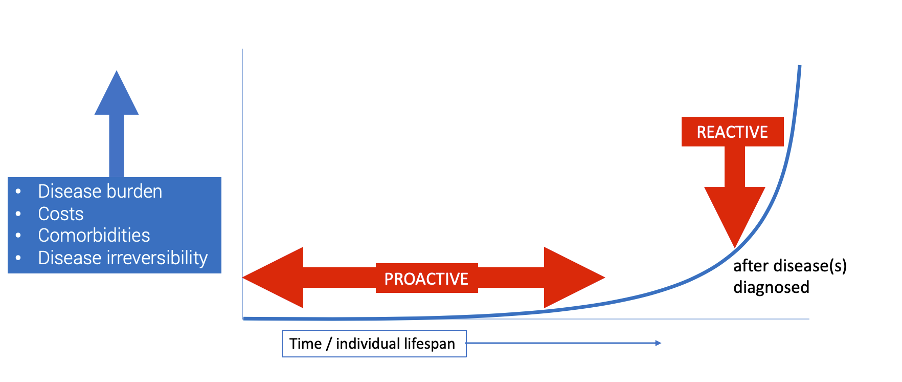
If the management of our health is to become sustainable, we must transition from a solely reactive model of healthcare to one that is also proactive, as proposed in the ANH-Intl blueprint.
The crash course we’ve been on for decades
The public has been fed information via the media that says that certain people – those with underlying illnesses such as hypertension, type 2 diabetes and lung disease – are especially vulnerable to severe covid disease. They say very little or nothing about how those who’re presently free from these diseases might stay free from them. Also, while we’re so completely focused on this pandemic – how much time do we spend considering how we might respond, physiologically, psychologically, psycho-socially, politically, economically and in other ways, if we were confronted with another virus, one more virulent and contagious than SARS-CoV-2? Yes, it doesn’t bear thinking about.
Rather than give you more words to read, we decided to create an infographic that depicts this crash course. In essence, it’s one in which the effects of a relatively innocuous virus has demonstrated its capacity to cause global mayhem – because we are insufficiently adapted to our modern world. It is also because the actions that were taken by governments and businesses were deemed to be of benefit by those interests that usurp most power in today’s deeply anthropocentric and often narcissistic world. Our thrifty, hunter-gatherer genotype doesn’t cope well with the onslaught of processed foods, physical inactivity, social disconnection, chemical pollution, information and digital overload, disturbed circadian cycles, and chronic, seemingly never-ending, stress.
How can we build resilience?
Resilience requires that multiple systems within what we call our ‘ecological terrain’ are working optimally. Our blueprint identifies 12 domains that, when the function of each is optimised, allows us to achieve optimal resilience. There is no one-size-fits-all. We are all individuals, with unique genotypes, each of which has been marked epigenetically according to the lives and environments we have experienced. These epi-marks dictate which of our genes are silenced and which are expressed – and, if so, by how much. Our gene expression pattern at any given point in time, determines our health and resilience, as well as our propensity for particular types of disease.
Dietary, lifestyle, behaviour and environmental changes provide the most potent ways available to us that allow us to change our pattern of gene expression. As much as pharmaceutical and vaccine interests might wish us to think differently, these kinds of changes are by far the most important preventive defences we have against this new coronavirus or any future infectious agent. They always have been and they always will be.
>>> Find out more about ANH-Intl’s blueprint for health system sustainability
Why the silence on resilience?
There is a simple answer to this question. The business model that has driven the shape and form of healthcare over the last 7 decades has to a large extent been one built on selling novel, new-to-nature compounds and technologies that are amenable to patents.
One industry alone cannot engage in health creation – so it’s been given a wide birth by pharma. Vaccination, on the other hand, particularly if indemnified by governments in the event of no-fault injury caused to those vaccinated, is a much more economically attractive proposition than creating what Leroy Hood PhD calls ‘scientific wellness’. However, as we propose in our blueprint, communities have the ability to build the physiological resilience of their populations, especially if they have a common language. Our blueprint outlines such a language as well as the practicalities of how this might be done, built around function and a systems view of human, other animal, plant and microbial life.
So let’s understand what’s happening and get on with the job of preventing further collisions like that of Covid-19 that result from our inadequate adaptation to the contemporary world. We need to adapt better ourselves, but equally, we must adapt the political and economic systems that presently exert so much control – often not in a good way – over both people and planet.
>>> Return to ANH-Intl homepage








Comments
your voice counts
09 August 2020 at 9:46 pm
Social and cultural iatrogenesis
The 20th-century social critic Ivan Illich broadened the concept of medical iatrogenesis in his 1974 book Medical Nemesis: The Expropriation of Health[23] by defining it at three levels.
First, clinical iatrogenesis is the injury done to patients by ineffective, unsafe, and erroneous treatments as described above. In this regard, he described the need for evidence-based medicine 20 years before the term was coined.[24]
Second, at another level social iatrogenesis is the medicalization of life in which medical professionals, pharmaceutical companies, and medical device companies have a vested interest in sponsoring sickness by creating unrealistic health demands that require more treatments or treating non-diseases that are part of the normal human experience, such as age-related declines. In this way, aspects of medical practice and medical industries can produce social harm in which society members ultimately become less healthy or excessively dependent on institutional care. He argued that medical education of physicians contributes to medicalization of society because they are trained predominantly for diagnosing and treating illness, therefore they focus on disease rather than on health. Iatrogenic poverty (above) can be considered a specific manifestation of social iatrogenesis.
Third, cultural iatrogenesis refers to the destruction of traditional ways of dealing with, and making sense of, death, suffering, and sickness. In this way the medicalization of life leads to cultural harm as society members lose their autonomous coping skills. It is worth noting that in these critiques "Illich does not reject all benefits of modern society but rejects those that involve unwarranted dependency and exploitation."[25]
https://en.wikipedia.org/wiki/Iatrogenesis
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences