Content Sections
By Meleni Aldridge, executive coordinator, ANH-Intl
As we discussed last week, the skyrocketing increase in autoimmune disease could soon eclipse heart disease, the no 1 killer in the Western world. We described the role that gluten plays, but we didn’t discuss gender or the contributory role emotions play in the development of an autoimmune disease. This week’s article is based on Dr Keesha Ewers’ brilliant lecture, Stress and Autoimmune Disease, at the Institute for Functional Medicine’s 2018 annual conference.
In short, if you’re a woman with a challenging emotional landscape, you are up to 10 times more at risk of developing certain autoimmune diseases – and you may know nothing about it for twenty to thirty years. Eighty percent of all autoimmune diseases diagnosed are in women and once the seal is broken so to speak, there is a 75% chance of developing more if the causes aren’t fully addressed.
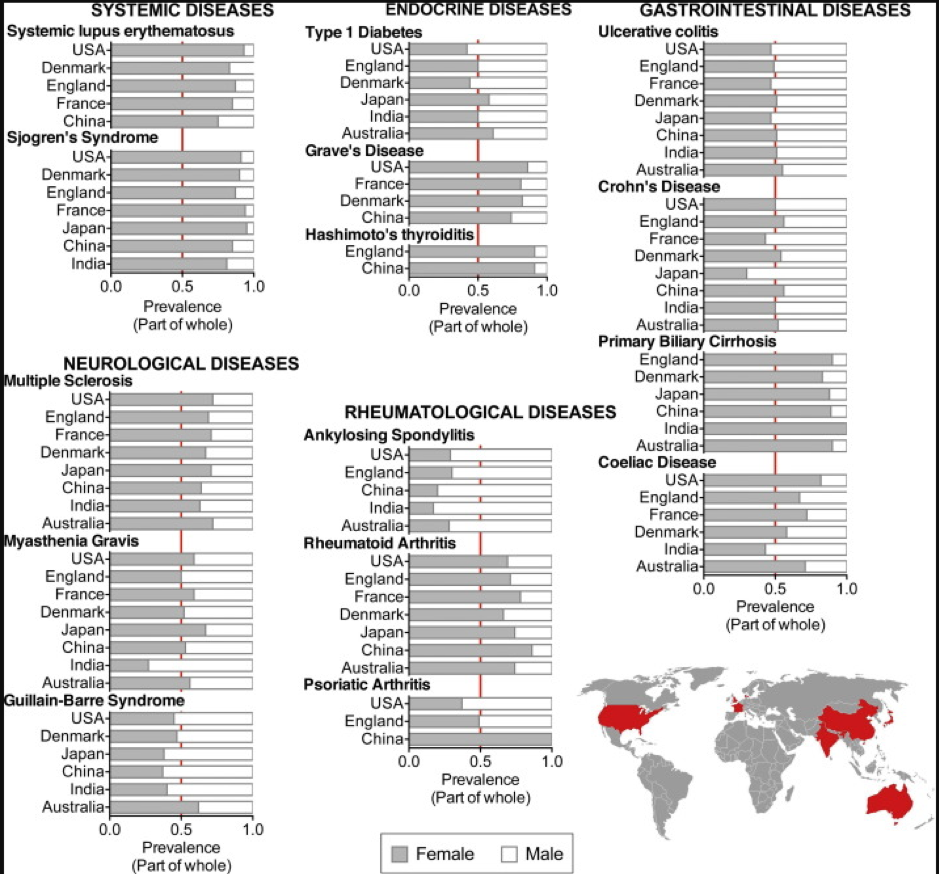
Figure. Gender difference in autoimmune disease.
Source: T. Ngo, F.J. Steyn, P.A. McCombe. Gender differences in autoimmune disease. Frontiers in Neuroendocrinology 2014; 35 (Issue 3): 347-36
The mind and body at war
There are no winners when the mind and body are at war. Our immune system is like the archer carrying a bow and a quiver of arrows. Everything works perfectly when it takes aim with one arrow at an identified target, but autoimmune problems occur when the quiver is emptied of arrows firing indiscriminately and continuously. This is what happens when early life trauma, chronic stress, unhappiness and heart pain keep the immune system triggered with no end in sight.
The brain communicates with the immune system through the autonomic nervous system and through hormonal activity. Both pathways generate signals that are perceived by the immune system via receptors on the surface of white blood cells and other immune cells. An activated immune system generates chemical messenger signals called cytokines that are in turn perceived by the nervous system. This two-way communication pathway connects the brain and the immune system with our hormones and our entire physiology, which is why it creates the foundation for behavioural influences on immune functions i.e. disease conditions.

Altering perceptions
If this is you, the first step is to recognise that your emotions affect your physical wellbeing and your physiology. You can’t be unhappy without your immune system responding in the same way as it does to an infection or a wound because it doesn’t differentiate between stressors. You may not be able to reduce your stress because we live in a stressful society and you may not know how to address what’s hurting you because it’s rooted in early life trauma. But you can reduce your perception (the way you feel) of that stress. Sometimes just knowing that allows you to breathe, pause and accept the ‘What Is’ of your life.
Early life trauma creates more tissue in the right hemisphere (the emotional side) of the brain, a denser and bigger amygdala (involved in experiencing emotions) and a more reactive, hair trigger stress response. This creates a physiological cascade, detailed above, that affects mood, inflammation, anxiety levels and can make one more prone to obesity. It can become a vicious circle if action isn’t taken to break the feedback loop.
As humans we are wired to experience rejection as trauma as it was our survival mechanism to prevent us straying outside of the tribe where we could get hurt or killed. As such, we have all experienced trauma at some time in our lives because we have all experienced rejection. However, the more adverse childhood experiences (ACE) someone has that are unresolved, the more symptoms will be experienced in the body. Additionally, the ability, or desire, to self-care – especially in women – reduces when the ACE score, or the perception of stress from the trauma, is high. Conversely, autoimmunity increases – the risk of hospitalisation with an autoimmune disease is 70-80% higher with an ACE score of 2 or more.
Steps to healing
Ask yourself, what do I need in order for my archer to put its bow and arrows down? Don’t censor the response you get, accept the first answer that arises no matter how absurd it may seem.
A hyper vigilant mind and immune system causes something that some practitioners refer to as a ‘pregnenalone steal’, which leads to hormone imbalance and a leaky gut. The way you feel about (perceive) your stress is what is important though, because we experience feelings first, which affect the brain. Hence, perceived chronic daily stress looks the same on the brain scans as someone with post-traumatic stress disorder (PTSD). The higher your perceived stress score, the worse the symptoms you may be experiencing – or brewing.
This is where mindfulness practices, meditation and heart rate variability training like the HeartMath Institute teach are very important. Victims don't heal, which is why one often needs to hit rock bottom before finding the motivation to choose healing.
Find out your Perceived Stress Score (PSS) by downloading the pdf below. (Please note you'll need to download the PDF into Adobe Reader or Pro to automate the form, as not all browsers support the functionality). Please ensure you use the interactive PDF to score yourself. Do not score yourself using the image below as you will get an incorrect score.
If you are scoring moderate to high stress, I recommend that you visit the links below in the self-care section, find what resonates with you, commit to a practice that fits with your life and take the quiz every few months to check your progress.
 Walking free
Walking free
Freedom comes from connecting the dots in our emotional landscape. Being brave enough to acknowledge the root(s) of our emotional pain, challenges and traumas and then looking clearly at our beliefs, behaviours, diet, mood and relationships. Once you’ve established your trauma timeline through the PSS and ACE questionnaires, you can acknowledge ‘What Is’. This is often the first step on the healing journey – from misery to motivation.
There are many self-care tools to help you find the eye in your hurricane when it hits – a place of calm and rebalancing to restore resilience. A few of them are below.
In my view, it's really important to remember that intention is one of the most powerful tools we all possess for self-healing. This is where techniques such as re-framing and forgiving allow us to confront ourselves, therein releasing trauma and experiencing hope again.
It’s also been shown that stress is ancestral (epigenetic) and can transfer across the generations, thus, our healing is not always solely for ourselves.
Solving The Autoimmune Puzzle with Dr Keesha Ewers
Additional Self-Help resources:
Find out your Adverse Childhood Experiences (ACE) score
Take the Perceived Stress Scale test (PSS), which can be repeated regularly to track your progress
Dr Keesha Ewers: Solving the Autoimmune Puzzle – The woman’s guide to reclaiming emotional freedom and vibrant health
Dr Keesha Ewers’ healing programmes
The HeartMath Institute resources for reducing stress and empowering you
Bessel van der Kolk MD: The Body Keeps the Score
Dr Vincent Felitti: Reflections on the Adverse Childhood Experiences (ACE) Study







Comments
your voice counts
There are currently no comments on this post.
Your voice counts
We welcome your comments and are very interested in your point of view, but we ask that you keep them relevant to the article, that they be civil and without commercial links. All comments are moderated prior to being published. We reserve the right to edit or not publish comments that we consider abusive or offensive.
There is extra content here from a third party provider. You will be unable to see this content unless you agree to allow Content Cookies. Cookie Preferences