Content Sections
- ● Introduction to the Test & Take campaign
- ● Why is vitamin D so important?
- ● What sets vitamin D aside from other hormones?
- ● Co-factors or ‘assistant nutrients’
- ● Why is vitamin D important for immune protection?
- ● Why are government levels too low for immune protection?
- ● Vitamin D science and covid-19
- ● How do I find my vitamin D level?
- ● What should my level be?
- ● How to optimise your vitamin D levels
- ● Additional resources
- ● Additional ‘D’ reading from the ANH archives
Government advice and public health messaging about the importance of vitamin D is woefully inadequate globally and where there is a suggestion that supplementation may be beneficial, the recommended levels are unlikely to make much of a difference to immune support.
A new study published yesterday (27th October 2020) confirms that more than 80 per cent of hospitalised covid-19 patients in Spain had vitamin D deficiency. This further backs up what was already shown a few months back in Italy.
Given the wealth of clinical data gleaned from the trauma of the past few months, we feel it imperative to launch this vitamin D campaign to help you support your immune system and protect yourself and your loved ones.
For those of us who are moving into the northern winter where our bodies can’t make its own vitamin D from sunlight, supplementation becomes essential. The bottom line is that government health authorities are still ignoring decades of published, peer reviewed research by vitamin D researchers and clinicians. We hope that the following information sets you on the path to effective vitamin D self-care.
Introduction to the Test & Take campaign
Video: what governments are and aren't telling us
The case for Vitamin D Supplementation - an interview with vitamin D expert, Dr Damien Downing
Note: You will see an advertising banner beneath our videos that play off the Brighteon platform (when they are not maximised). This advertising helps support the Brighteon platform that doesn't charge subscribers for their content, is committed to free speech, yet is also respectful of copyright-related law. We'd like to clarify that no advertising revenue from Brighteon is received by the Alliance for Natural Health Intl.
Why is vitamin D so important?
The importance of vitamin D for our health and well being cannot be underestimated. In fact, it’s absolutely essential for life and plays a vital a role in a multitude of our bodies’ functions. Vitamin D is literally involved in thousands of genetic and metabolic processes and almost every cell needs it.
We need adequate levels for the proper functioning of our immune systems, strong bones and teeth, cancer prevention, reducing the risk of developing heart disease or autoimmune disease, modulation of inflammation and much more in terms of lowering the risk of disease.

Unfortunately, with the rise in the use of sunscreens and increased fear of the sun, vitamin D blood levels have plummeted globally. Around 40-75% of the world’s population are now estimated to be vitamin D deficient. Not so much as to cause the deficiency disease, Rickets, but enough to interfere with health, normal function and protection against disease. Such is the scale of the problem, it’s now considered to be a global public health issue, yet still we see such reluctance on the part of health authorities to take much-needed action.
What sets vitamin D aside from other hormones?
Technically vitamin D is not a vitamin in the true sense as we don’t obtain what we need from our food, or make it in our gut. It is in fact a pro-hormone that is produced in our skin when we expose enough of our body to sunlight. This makes total sense when you consider the importance of vitamin D to our health and the potential for famine during human evolution. Our hunter gatherer ancestors didn’t cover their bodies the way we do now, which left over 80% of skin bare to synthesize vitamin D. As we evolved near to the equator, this was a failsafe way to ensure vitamin D levels would always be adequate.
Despite being very different, vitamin D is still classified as one of four (A, D, E and K) fat-soluble vitamins. Named such as these vitamins require fat for effective absorption as they don’t dissolve in water.
Did you know that your body can produce 10,000 to 25,000 IU (250 – 625mcg) of vitamin D in around 15-20 mins of sun exposure at the height of the midday summer sun? This is just under the time that even the most sensitive skins will burn, making it achievable for most people.
When sun exposure is not an option, for any reason, supplementation is the next best choice. Vitamin D, whether it’s made in your skin through exposure to sunlight or taken as a supplement, is then converted by your liver to a form called 25-hydroxyvitamin D, written in the short form as 25(OH)D. In order for it to be in a form that your body can use, it must then go through a second process in the kidneys to make the biologically active form of vitamin D, called 1,25-dihydroxyvitamin D, or 1,25(OH)2D.
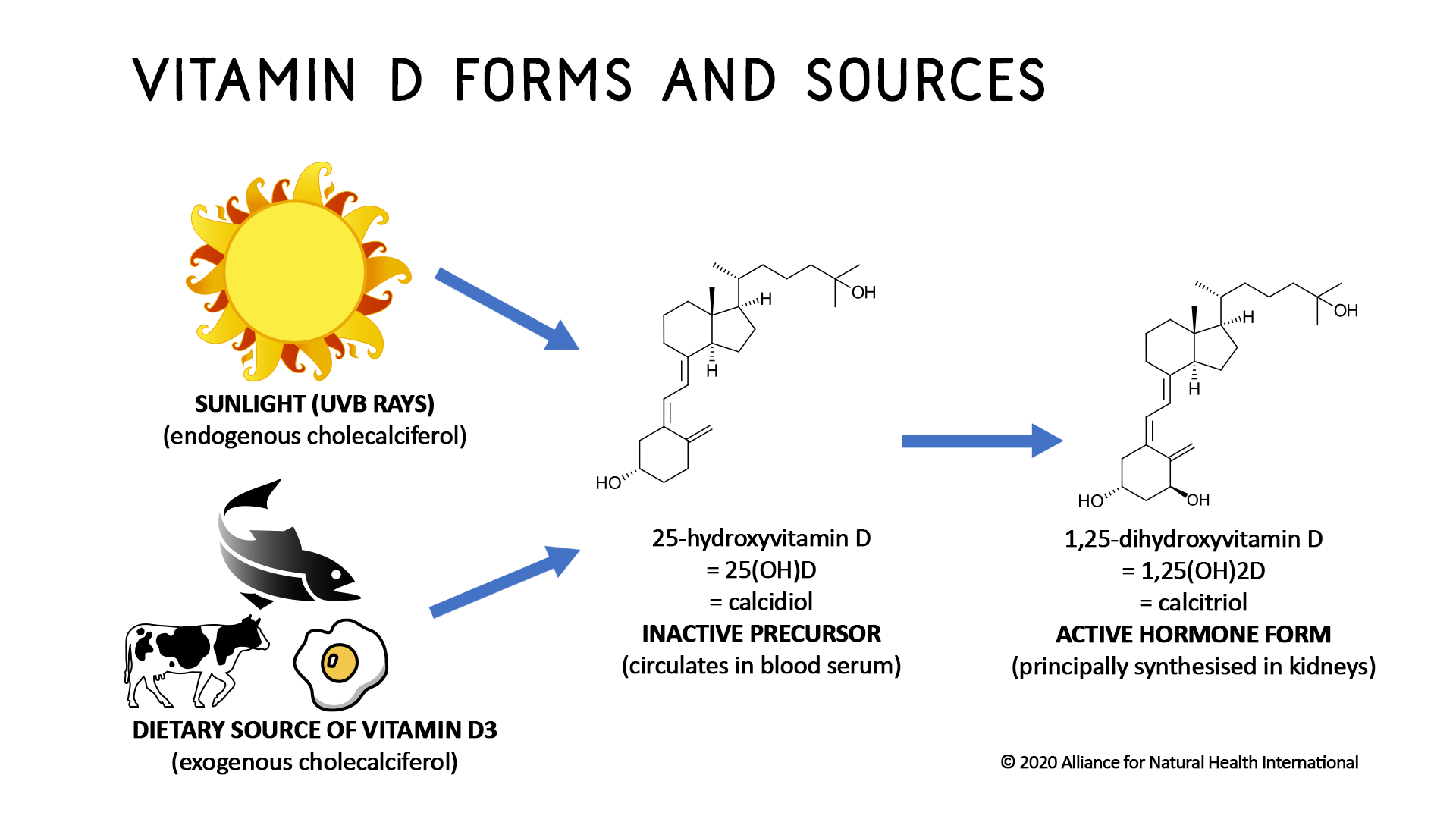
The elderly, people with darker skin tone, those who are are overweight/obese or live in areas where there is limited sunlight have a much higher risk of becoming deficient in vitamin D.
Co-factors or ‘assistant nutrients’
This conversion is dependent on a number of co-factors or ‘assistant nutrients’, meaning that we also need adequate levels of magnesium, boron, zinc, vitamins A, K2 and B6, as well as omega 3 fatty acids. The latter helps the conversion to the active form of vitamin D (1,25(OD)2D), particularly for those with under-functioning liver or kidneys. These nutrients don’t only assist the conversion of vitamin D to the active form, they also help to make it more bioavailable and prevent the effects of overload.
Magnesium-rich foods include dark leafy greens, pulses (legumes), avocado, bananas, figs, strawberries, blackberries, nuts, seeds, brown rice, and dark chocolate. However, it’s often hard these days to get sufficient from foods alone, so supplementing with 500 - 750 mg per day of magnesium is beneficial when taking vitamin D3 in doses above 4,000 IU. Luckily, legumes, nuts and avocados are also good sources of boron.
Zinc isn’t just a helpful co-factor for vitamin D synthesis, but is also involved in over 300 enzymatic reactions in the body. It is very much an essential mineral and is found in red meat, shellfish, legumes, nuts and seeds.
Vitamin A as retinol is found in animal proteins and organ meats, but also in brightly coloured fruits and vegetables as beta-carotene.
Vitamin K2 is found in fermented foods and animal proteins, but can also be made in our bodies from vitamin K1, found in dark green leafy veg, particularly those from the cruciferous family (e.g. Brussels sprouts, broccoli, kale, spinach, chard). However, this depends greatly on the health of your gut and your microbiome. If you have issues in this area, then you can also supplement with vitamin K2. GrassrootsHealth recommends 90 mcg for women and 120 mcg for men daily.
There are also other co-factors and nutrients required to help maintain sufficient energy both for vitamin D metabolism and proper function of the immune system. Critical amongst these are vitamins B6, folate and B12. Both B6 and B12 especially the latter, are often found to be particularly limited among vegetarians and vegans.
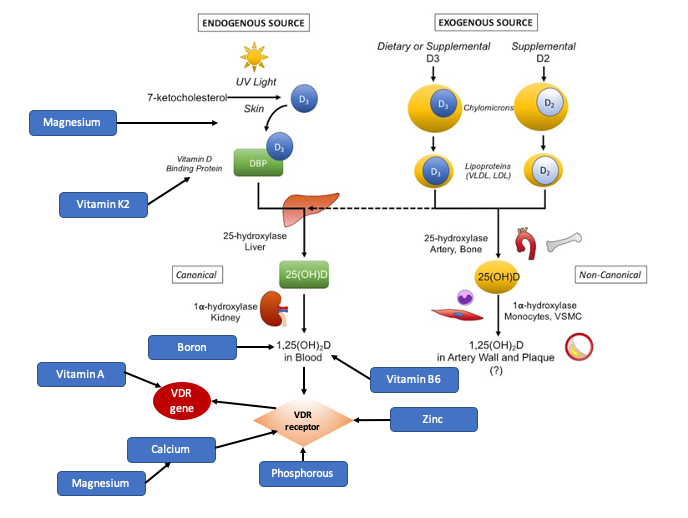
Vitamin D pathways and co-factors. Source: Adapted from Demer LL, Hsu JJ, Tintut Y. Steroid Hormone Vitamin D: Implications for Cardiovascular Disease. Circ Res. 2018 May 25;122(11):1576-1585
Why is vitamin D important for immune protection?
Vitamin D plays a critical role in promoting a robust and resilient immune system, which is our first line of defence against infection and disease.
Did you know that almost every cell involved in immune function contains a vitamin D receptor?.
Our immune system has two sides both of which are needed to fight infections. The innate system (our rapid response first line defence, which quickly responds to infections) and the adaptive system (which produces a slower response and is responsible for remembering previous invaders against which it produces antibodies and specialised resources to more quickly counter reinfection).
Low levels of vitamin D have been linked to an increased risk of acute respiratory infections, particularly in the elderly who are at much higher risk of becoming deficient.
Why are government levels too low for immune protection?
The majority of government recommendations for vitamin D intake are related to bone and musculoskeletal health.
Table 1. Government recommendations for Vitamin D supplementation by country.
|
Country |
Daily recommended vitamin D intake |
|
10 mcg (400 IU) |
|
|
15 mcg (600 IU) |
|
|
10 mcg (400 IU) |
|
|
5-10 mcg (200-400 IU) |
|
|
15 mcg (600 IU) |
|
|
20 mcg (800 IU) |
|
|
15 mcg (600 IU) |
|
|
50 mcg (2,000 IU) |
|
|
12.5 mcg (500 IU) |
Some governments are starting to recognise the importance of vitamin D supplementation for population heatlth.
- Israel started recommending vitamin D in October 2020.
- Slovenia has begun administering vitamin D to residents of nursing homes and health care workers.
- The French National Academy of Medicine recommends that people over 60 be tested for vitamin D deficiency and given a bolus dose of 50,000 to 100,000 IU. It further recommends that all Covid positive patients take 800 to 1000 IU a day upon diagnosis.
- A Swiss expert panel recommends that people supplement with 2,000 IU of vitamin D per day.
- New Zealand provides 50,000 IU monthly vitamin D supplementation to all aged care residents.
- The Scottish government will provide vulnerable populations with vitamin D supplementats
Vitamin D science and covid-19
Interest in vitamin D and its effects on our health has grown in recent years and its impact on a variety of health conditions. Despite the growing body of evidence pointing to vitamin D’s role in supporting our immune function and protecting us against infectious diseases it’s use as both a preventative and acute treatment for Covid-19 has been routinely dismissed by governments and health authorities alike. This wholesale dismissal has resulted in a raft of new studies being published in recent months supporting the role of vitamin D in countering the coronavirus.
A number of studies have now shown those who are vitamin D deficient were much more likely to have covid than those who weren’t. They were also at high risk of developing severe illness from covid-19 leading to the need for mechanical ventilation and/or death. Another study from researchers in Israel also found a link between low levels of plasma (25(OH) vitamin D and increased risk of infection by SARs-CoV-2 the virus responsible for covid-19.
Such is the interest in the association between low levels of vitamin D and covid-19, that there are now approximately 30 different clinical trials taking place to test the effectiveness of vitamin D supplementation to prevent and treat the disease. Researchers at Queen Mary University of London are looking for 5,000 UK residents to take part in a new study, CORONAVIT, to find out if supplementing with vitamin D can protect people from catching covid-19.
A recent review found vitamin D deficiency was common worldwide echoing previous findings.
Data on the effect of vitamin D in relation to prevention of covid-19 are scarce, but one study has reported the active form of vitamin D (1,25-dihydroxyvitamin D) inhibits SARS-CoV-2 in the nasal cells.
The majority of testing looks at 25(OH)D as a marker of vitamin D status with low levels being associated with a range of diseases, however a recent study suggests the active form of vitamin D, 1,25(OH)2D, is a better marker of vitamin D status.
There is now broad consensus that vitamin D has a role to play in both prevention and treatment of respiratory illness including against SARS-CoV-2. What is still to be determined is the optimal range for supplementation with vitamin D given the majority of government recommendations are aimed at supporting bone and musculoskeletal health rather than supporting immunity.
A small study of covid-19 patients found a high dose of 50,000 IU (1,250 mcg) vitamin D daily for 5 days normalised vitamin D levels and improved recovery time more effectively than a lower dose of 1,000 IU (25 mcg) daily. A combination of magnesium (150 mg/d), vitamin B12 (500 mg/d) and vitamin D (1,000 IU/d) administered to older patients admitted to hospital was found to reduce the likelihood of them requiring ventilation or intensive care support. Magnesium is recognised as an important co-factor for the effective metabolism of vitamin D along with vitamin K2, which helps control the amount of vitamin D made by the body, while zinc helps the body to utilise vitamin D.
Researchers publishing in Nutrition recommend those at higher risk of developing respiratory infections including covid-19 should take 10,000 IU/d (250 mcg) of vitamin D for a few weeks to raise 25(OH)D levels above 40-60 ng/ml (100-150 nmol/l) followed by a maintenance dose of 5,000 IU/d (125 mcg). They also suggest higher doses may be useful as part of a treatment protocol for those infected with covid-19.
A recent white paper from an expert panel of doctors and scientists working with the Swiss Society of Nutrition recommends a standard dose of 2,000 IU/d (50 mcg) as part of a protocol to support the immune system, particularly in adults over the age of 65. The recommended dose is higher than the daily recommended intake of 800 IU (20 mcg), which has been shown to be protective against respiratory infections, but is well below the tolerable upper limit of 4,000 IU/d.
How do I find my vitamin D level?
Our individual vitamin D requirements vary hugely and there’s no clear correlation between circulating blood serum levels and intake. It’s down to uptake in the body rather than intake that’s important. The amount an individual needs is dependent on their age, race, lifestyle, where they live and genetic make-up. In some people gene copying errors through single nucleotide polymorphisms (SNPs) can make vitamin D receptors less sensitive meaning they need a higher intake than others. You can take a genetic test to check for polymorphisms if you find you’re struggling to optimise your vitamin D levels.
The only way to determine how much you need is to take a test. If you’re in the UK it’s unlikely you will be able to access testing through your NHS GP unless you’re showing signs of serious disease such as osteomalcia. That is no longer an issue as there are a number of DIY home testing kits available and more coming onto the market regularly. Below is a small selection of tests available in the UK.
Table 2. Examples of some UK-based vitamin D home testing companies.
|
Company |
Type of test |
Cost |
|
Kiweno DIY Vitamin D test (- your numerical result is available via your smart phone in approx. 15 mins) |
Fingerprick bloodspot |
£39.99* |
|
Fingerprick bloodspot |
£39.00 |
|
|
VitaminDtest.org.uk (NHS pathology lab) |
Fingerprick bloodspot |
£29.00 |
|
Fingerprick bloodspot |
£39.00 |
|
|
Better You (- includes vitamin D spray) |
Fingerprick bloodspot |
£32.95 |
|
Vitamin D Rapid Test Cassette (- range-based test gives you one of three results: deficient, insufficient and sufficient {no numerical level}, result in approx. 10 mins; no shipping fee for UK and Northern Ireland) |
Fingerprick bloodspot |
£7.95 |
>>> NB: If you’re not based in the UK, please search for ‘Vitamin D bloodspot home test kit’ in your own country or ask your doctor. In the US, vitamin D test kits can be obtained from GrassrootsHealth.
GreenVits is a campaign partner and supporter of ANH-Intl. Use the code ANH10 on purchases of vitamin D supplements to receive a 10% discount and gift an additional 5% donation to ANH-Intl.
We've tested our own vitamin D levels here at the office using the Kiweno rapid test and created a short video to show you the steps. As you see, this member of our team needs to get their vitamin D levels up! The fingerprick tests are all quite similar and are very easy to do at home.
Note: You will see an advertising banner beneath our videos that play off the Brighteon platform (when they are not maximised). This advertising helps support the Brighteon platform that doesn't charge subscribers for their content, is committed to free speech, yet is also respectful of copyright-related law. We'd like to clarify that no advertising revenue from Brighteon is received by the Alliance for Natural Health Intl.
Using a questionnaire-based app to check your levels
If it's not possible for you to purchase a test, then you can still get some idea of where your level might be by using the D Minder Pro app from the App Store and the D Minder app from Playstore. The app is expertly designed to help you track and manage your vitamin D levels and is free till the end of the year because of the pandemic. We'd also recommend its use even if you are testing as it's a handy, low cost, method of keeping track in between tests, as well as providing you other useful data related to your geographical location.
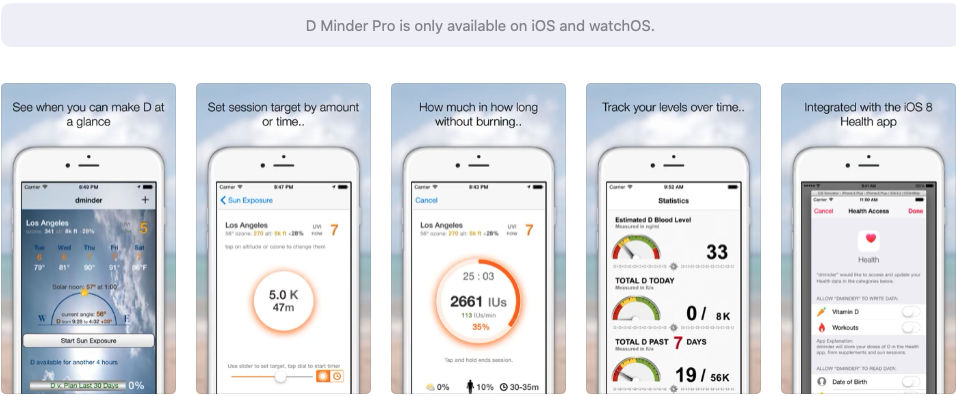
What should my level be?
The minimal 10-15 micrograms or 400-600 International Units per day recommended by most governments is barely enough to stave off the deficiency disease, Rickets. This is why vitamin D researchers and experienced clinicians recommend 100 to 125 micrograms or 4000 to 5000 International Units as a daily maintenance dose in the absence of sunlight exposure, with higher levels short term when you have an immune challenge.
Dr Damien Downing, president of the British Society for Ecological Medicine and vitamin D expert, recommends a vitamin D blood level of at least 75 nmol/L for immune support and levels over 100 nmol/L to lower your risk of cancer and autoimmune disease.
When talking doses, let’s bear in mind that just 20 minutes with 80% of your body exposed to a midday, midsummer sun in a typical northern latitude will give you circulating levels of vitamin D that are equivalent to taking around 500 micrograms or 20,000 International Units of vitamin D3.
Table 3. Comparison levels between conventional medicine and the Vitamin D Global Expert Group in nmol/L.
|
Source |
Deficient |
Insufficient |
Adequate |
Optimal |
Reference |
|
NHS (UK) |
<25 |
25-50 |
>50 |
N/A |
|
|
Exeter Clinical Lab (NHS) |
<10 |
10-35 |
36-60 |
>60 |
|
|
Grassroots Health (vitamin D global expert group) |
<100 |
<100 |
<100 |
100-150 |
Please note that there are two different measurement units used for assessing serum levels of 25-hydroxyvitamin D. The United States uses measurements of nanograms per millilitre (ng/ml) and the UK, Canada and Europe uses nanomoles per litre (nmol/L). Therefore target levels that are beneficial for health range from 40 - 60 ng/ml or 100 - 150 nmol/L depending on which test you are using or where you are in the world.
How to optimise your vitamin D levels
Once you've determined your levels as best you can - either with a test kit or by using one of the D Minder apps - use the charts below to guide your supplementation level.
If you find that your serum 25-hydroxyvitamin D level is low or very low, we'd always recommend working with a qualified health professional to individualise your supplement plan. We are busy compiling a list of practitioners in the UK who are signing on to partner this campaign, but you can also refer to The Institute for Functional Medicine's Find a Practitioner Section, which is international, or in the UK, refer to The British Society for Ecological Medicine.
Supplementing with vitamin D
When considering supplementing with vitamin D, you need to know that vitamin D isn't just one single vitamin, but a family of nutrients with similar chemical structures. The forms of vitamin D most commonly found in the diet are D2 (ergocalciferol) from plant foods like mushrooms and D3 (cholecalciferol) from foods like fatty fish, fish oils, eggs, butter and liver. Apart from not really being able to eat enough to bring your vitamin D levels into the optimal range without sun exposure, vegans and vegetarians are more at risk of not getting enough D3, which the main circulating form and the one that your skin makes from the sun.
Research has shown that whilst both forms are effectively absorbed into the bloodstream, differences in the way the liver breaks them down means that D2 doesn't raise your serum blood levels as well as D3. For this reason, most clinicians and researchers will recommend taking vitamin D3, cholecalciferol, as a supplement and there are now vegan forms available too. Many of the existing vitamin D3 supplements come from lanolin in sheeps' wool.
As D2 is much cheaper to make you'll find it in fortified foods and in some supplements. It's also vegan, but bear in mind that you will have to take significantly more, possibly twice the amount of D3, to raise your circulating level of vitamin D.
There are many supplements on the market that combine vitamin D3 with additional co-factors like vitamin K2. This is completely understandable, but our suggestion is that you purchase D3 as a single nutrient so that you can optimise your dose for your individual requirements as necessary without necessarily raising the levels of the other nutrients. You then still have the option of taking the product with the additional co-factors, but have the extra D3 on it's own if you need to take more.
Regular testing every 3 months is always advisable (or use of the DMinder app) and even more so when you've tested low and need to optimise. The charts below from GrassrootsHealth are the result of decades of work by vitamin D experts. We've included them as a guideline for optimising your supplement dose if you find your levels of vitamin D are too low. The two charts contain the same information, but defined by the different units of measurements, i.e. nmol/L and ng/ml.

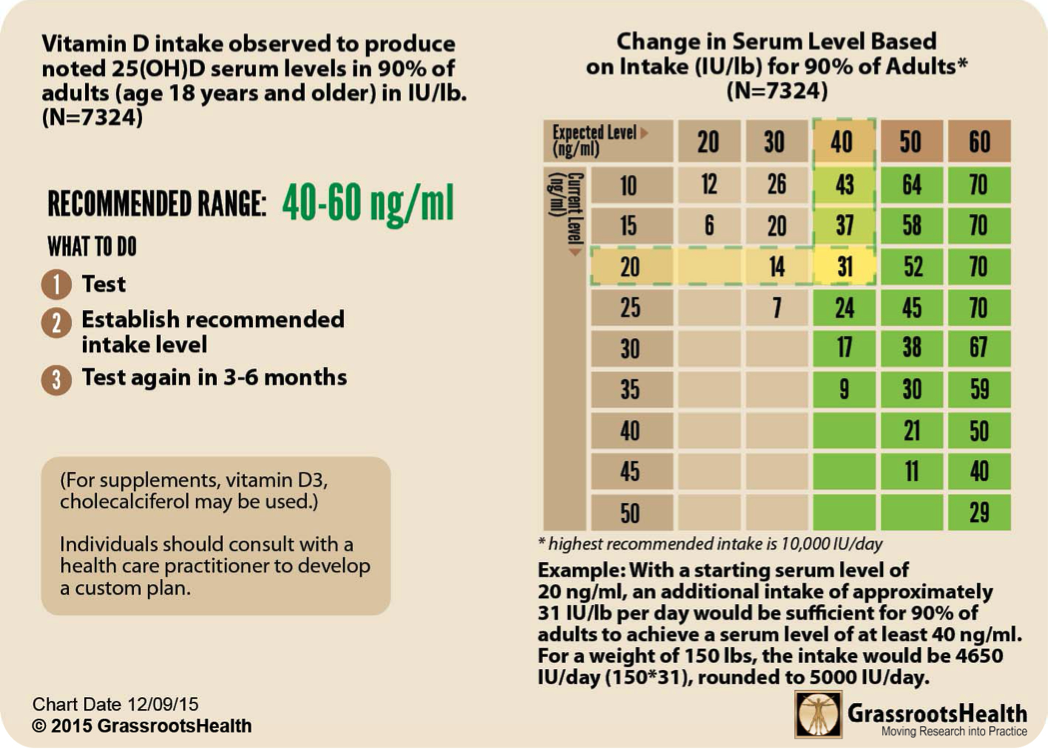
A guideline for vitamin D supplementation dosages for children (age 4-17) and adults
|
Age group |
Daily dosage of vitamin D |
|
Children (4-6 years) |
20-25 micrograms (800-1000 IU) |
|
Children (7-10 years) |
25 micrograms (1000 IU) |
|
Teens (10-17 years) |
50 micrograms (2000 IU) |
|
Young adults (18 years and over) |
100 micrograms (4000 IU) |
Additional resources
Facts about Vitamin D and Coronavirus
Improve health immunity for all now - sign the petition
Additional ‘D’ reading from the ANH archives
Sunday Times late-winter attack on high dose vitamin D [26 Feb 2020]
Let’s beat the vitamin D pandemic before it beats us! [28 Aug 2019]
Are you rea’D’y for Winter? [22 Nov 2018]
Vitamin D - Prevention rather than cure [16 Aug 2017]
UK government stays in the shade with no changes in vitamin D recommendations [12 Aug 2015]
>>> Return to the ANH homepage






